|   An official website of the United States government The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site. The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely. - Publications
- Account settings
- My Bibliography
- Collections
- Citation manager
Save citation to fileEmail citation, add to collections. - Create a new collection
- Add to an existing collection
Add to My BibliographyYour saved search, create a file for external citation management software, your rss feed. - Search in PubMed
- Search in NLM Catalog
- Add to Search
The Top 100 Cited Articles in Clinical Orthopedic Sports MedicineAffiliation. - 1 Department of Orthopaedic Surgery, The Johns Hopkins University, Baltimore, MD. [email protected].
- PMID: 26251939
Orthopedic sports medicine continues to evolve, owing much of its clinical management and practice to rigorous academic research. In this review, we identify and describe the top 100 cited articles in clinical sports medicine and recognize the authors and institutions driving the research. We collected articles (excluding basic science, animal, and cadaveric studies) from the 25 highest-impact sports medicine journals and analyzed them by number of citations, journal, publication date, institution, country, topic, and author. Mean number of citations was 408 (range, 229-1629). The articles were published in 7 journals, most in the 1980s to 2000s, and represented 15 countries. Thirty topics were addressed, with a heavy emphasis on anterior cruciate ligament injury and reconstruction, knee rating systems, rotator cuff reconstruction, and chondrocyte transplantation. The 3 most cited articles, by Insall and colleagues, Constant and Murley, and Tegner and Lysholm, addressed a knee, a shoulder, and another knee rating system, respectively. Several authors contributed multiple articles. The Hospital for Special Surgery and the University of Bern contributed the most articles (5 each). This study provides a comprehensive list of the past century's major academic contributions to sports medicine. Residents and fellows may use this list to guide their scholarly investigations. PubMed Disclaimer Similar articles- The fifty highest cited papers in anterior cruciate ligament injury. Vielgut I, Dauwe J, Leithner A, Holzer LA. Vielgut I, et al. Int Orthop. 2017 Jul;41(7):1405-1412. doi: 10.1007/s00264-017-3513-3. Epub 2017 May 27. Int Orthop. 2017. PMID: 28550427
- Fifty most cited articles in orthopedic shoulder surgery. Namdari S, Baldwin K, Kovatch K, Huffman GR, Glaser D. Namdari S, et al. J Shoulder Elbow Surg. 2012 Dec;21(12):1796-802. doi: 10.1016/j.jse.2011.11.040. Epub 2012 Apr 7. J Shoulder Elbow Surg. 2012. PMID: 22484389 Review.
- Italian research on anterior cruciate ligament: a bibliometric analysis. D'Ambrosi R, Migliorini F, Di Maria F, Anghilieri FM, Di Feo F, Ursino N, Mangiavini L, Kambhampati SBS. D'Ambrosi R, et al. Eur J Orthop Surg Traumatol. 2024 Jul;34(5):2235-2243. doi: 10.1007/s00590-024-03937-3. Epub 2024 Apr 11. Eur J Orthop Surg Traumatol. 2024. PMID: 38602582 Review.
- Citation classics in radiology journals: the 100 top-cited articles, 1945-2012. Yoon DY, Yun EJ, Ku YJ, Baek S, Lim KJ, Seo YL, Yie M. Yoon DY, et al. AJR Am J Roentgenol. 2013 Sep;201(3):471-81. doi: 10.2214/AJR.12.10489. AJR Am J Roentgenol. 2013. PMID: 23971438
- The 25 most cited articles in arthroscopic orthopaedic surgery. Cassar Gheiti AJ, Downey RE, Byrne DP, Molony DC, Mulhall KJ. Cassar Gheiti AJ, et al. Arthroscopy. 2012 Apr;28(4):548-64. doi: 10.1016/j.arthro.2011.08.312. Epub 2012 Jan 20. Arthroscopy. 2012. PMID: 22265048
- Publications and ranking in orthopaedics and sports medicine of European countries during the last three decades: A bibliometric analysis. Vaishya R, Vaish A, Schäfer L, Migliorini F. Vaishya R, et al. J Orthop. 2024 Jul 3;58:96-101. doi: 10.1016/j.jor.2024.07.002. eCollection 2024 Dec. J Orthop. 2024. PMID: 39100540
- Bibliometric Analysis of Top 100 Systematic Reviews and Meta-analyses in Orthopaedic Literature. Banerjee S, Khatri N, Kaur A, Elhence A. Banerjee S, et al. Indian J Orthop. 2022 Feb 3;56(5):762-770. doi: 10.1007/s43465-022-00604-9. eCollection 2022 May. Indian J Orthop. 2022. PMID: 35547342 Free PMC article. Review.
- Top 50 Cited Bone Graft Orthopedic Papers. Elshohna M, Tsouklidis N. Elshohna M, et al. Cureus. 2022 Mar 23;14(3):e23419. doi: 10.7759/cureus.23419. eCollection 2022 Mar. Cureus. 2022. PMID: 35481294 Free PMC article. Review.
- A Bibliometric Analysis of the Top Cited Articles in Sports and Exercise Medicine. Khatra O, Shadgan A, Taunton J, Pakravan A, Shadgan B. Khatra O, et al. Orthop J Sports Med. 2021 Jan 22;9(1):2325967120969902. doi: 10.1177/2325967120969902. eCollection 2021 Jan. Orthop J Sports Med. 2021. PMID: 33553441 Free PMC article.
- The impact of the 30 most cited articles on hip arthroscopy: what is the subject matter? von Glinski A, Yilmaz E, Goodmanson R, Pierre C, Frieler S, Shaffer A, Ishak B, Lee CB, Mayo K. von Glinski A, et al. J Hip Preserv Surg. 2020 Feb 24;7(1):14-21. doi: 10.1093/jhps/hnz067. eCollection 2020 Jan. J Hip Preserv Surg. 2020. PMID: 32382424 Free PMC article.
Publication typesLinkOut - more resources- MedlinePlus Health Information
Miscellaneous- NCI CPTAC Assay Portal
- Citation Manager
NCBI Literature Resources MeSH PMC Bookshelf Disclaimer The PubMed wordmark and PubMed logo are registered trademarks of the U.S. Department of Health and Human Services (HHS). Unauthorized use of these marks is strictly prohibited.  An official website of the United States government The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site. The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely. - Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now . - Advanced Search
- Journal List
- Sports (Basel)
 Physical Activity and Sports—Real Health Benefits: A Review with Insight into the Public Health of SwedenChrister malm. 1 Sports Medicine Unit, Department of Community Medicine and Rehabilitation, Umeå University, 901 87 Umeå, Sweden; [email protected] Johan JakobssonAndreas isaksson. 2 Department of Molecular Medicine and Surgery, Karolinska Institutet, 171 77 Solna, Sweden; [email protected] Positive effects from sports are achieved primarily through physical activity, but secondary effects bring health benefits such as psychosocial and personal development and less alcohol consumption. Negative effects, such as the risk of failure, injuries, eating disorders, and burnout, are also apparent. Because physical activity is increasingly conducted in an organized manner, sport’s role in society has become increasingly important over the years, not only for the individual but also for public health. In this paper, we intend to describe sport’s physiological and psychosocial health benefits, stemming both from physical activity and from sport participation per se. This narrative review summarizes research and presents health-related data from Swedish authorities. It is discussed that our daily lives are becoming less physically active, while organized exercise and training increases. Average energy intake is increasing, creating an energy surplus, and thus, we are seeing an increasing number of people who are overweight, which is a strong contributor to health problems. Physical activity and exercise have significant positive effects in preventing or alleviating mental illness, including depressive symptoms and anxiety- or stress-related disease. In conclusion, sports can be evolving, if personal capacities, social situation, and biological and psychological maturation are taken into account. Evidence suggests a dose–response relationship such that being active, even to a modest level, is superior to being inactive or sedentary. Recommendations for healthy sports are summarized. 1. IntroductionSport is a double-edged sword regarding effects on health. Positive effects are achieved primarily through physical activity, which is the main part of most sports. Many secondary effects of sport also bring health benefits, such as psychosocial development of both young [ 1 ] and old [ 2 ], personal development [ 3 ], later onset, and less consumption of alcohol [ 4 , 5 ]. Finally, those who play sports have a higher level of physical activity later in life [ 6 ], and through sport, knowledge of nutrition, exercise, and health can be developed [ 7 ]. Negative effects include the risk of failure leading to poor mental health [ 8 , 9 ], risk of injury [ 10 , 11 ], eating disorders [ 12 ], burnout [ 13 ], and exercise-induced gastrointestinal tract discomfort [ 14 ]. In sport, there are unfortunately also reports of physical and psychological abuse [ 15 ]. Negative aspects are more common in elite-level sports, where there is a fine balance between maximum performance and negative health. A somewhat unexpected effect of sport participation is that people submitting to planned training in some cases perform less physical activity compared to those who are exercising without a set schedule. One explanation can be a reduced spontaneous physical activity in the latter group [ 16 ]. Because physical activity is increasingly executed in an organized manner [ 17 , 18 , 19 ], sport’s role in society has become increasingly important over the years, not only for the individual but also for public health. In this paper, we describe the health effects of sport from a physiological and psychological perspective, related both to physical activity and added values of sport per se. Initially, brief definitions of various concepts related to physical activity and health are given. This is then followed by: (1) A brief description of how physical activity and training affect our body from a physiological perspective; (2) a report on the health effects of physical activity and training; and (3) sport’s specific influences on the various dimensions of health. We chose to discuss the subject from an age-related perspective, separating children/adolescents, adults, and the elderly, as well as separating for sex in each age group. 2. Definitions of Physical Activity, Exercise, Training, Sport, and HealthDefinitions and terms are based on “Physical activity in the prevention and treatment of disease” (FYSS, www.fyss.se [Swedish] [ 20 ]), World Health Organization (WHO) [ 21 ] and the US Department of Human Services [ 22 ]. The definition of physical activity in FYSS is: “Physical activity is defined purely physiologically, as all body movement that increases energy use beyond resting levels”. Health is defined according to the World Health Organization (WHO) as: “[…] a state of complete physical, mental and social wellbeing and not merely the absence of disease or infirmity” [ 21 ]. Physical activity can occur spontaneously (leisure/work/transport) or organized and be divided according to purpose: Physical exercise is aimed primarily at improving health and physical capacity. Physical training is aimed primarily at increasing the individual’s maximum physical capacity and performance [ 23 ]. Physical inactivity is described as the absence of body movement, when energy consumption approximates resting levels. People who do not meet recommendations for physical activity are considered physically inactive and are sometimes called “sedentary”. Sport can be organized by age, sex, level of ambition, weight or other groupings [ 24 ]. Sport can also be spontaneous [ 7 , 17 ] and defined as a subset of exercises undertaken individually or as a part of a team, where participants have a defined goal [ 7 ]. General recommendations for physical activity are found in Table 1 , not considering everyday activities. One can meet the daily recommendations for physical activity by brief, high-intensity exercise, and remaining physically inactive for the rest of the day, thereby creating a “polarization” of physical activity: Having a high dose of conscious physical training, despite having a low energy expenditure in normal life due to high volumes of sedentary time. Polarization of physical activity may lead to increased risk of poor health despite meeting the recommendations for physical activity [ 25 , 26 , 27 ]. During most of our lives, energy expenditure is greater in normal daily life than in sport, physical training, and exercise, with the exceptions of children and the elderly, where planned physical activity is more important [ 28 ]. Recommendations regarding physical activity for different target groups. Note that additional health effects can be achieved if, in addition to these recommendations, the amount of physical activity increases, either by increasing the intensity or duration or a combination of both. | Target Group | Recommendations | Purpose |
|---|
| All children and adolescents are recommended at least 60 minutes daily physical activity. Longer is better.
The physical activity should be primarily of aerobic nature and the intensity moderate (easy/medium pulse increase) to high (marked pulse increase).
Aerobic physical activity at high intensity at least 3 times a week.
Muscle-strengthening physical activity 3 times a week.
Weight-bearing activity, such as running and jumping, is positive for bone mineral density.
The physical activity level will gradually be adapted to the individual’s biological and psychosocial maturation. | Development of muscles and skeletal and nervous system.
Maintain a healthy weight and a good mental health.
Social development, integration, good self-esteem, and self-confidence.
Enhanced learning ability.
Recommendations are universal, but for individuals with illness, there may be special recommendations. |
| All adults from 18 years of age and above are recommended to be aerobically physically active at least 150 minutes a week at a moderate intensity (medium pulse increase), or at least 75 minutes per week at vigorous intensity (marked pulse increase).
The activities should be distributed over at least three separate days.
Muscle-strengthening physical activity at least twice a week should be performed. | Improvements in aerobic work capacity and muscle strength.
Recommendations are universal, but for individuals with illness, there may be special recommendations.
Profits from carrying out the activity are lower risk of disease, such as disturbed metabolism and certain cancers and bone fractures. |
| Same recommendations as adults.
Muscle strengthening exercises should be performed at a high velocity, if possible.
Balance training should be incorporated prior to aerobic and muscle strengthening training.
Individuals with impaired ability should perform as much exercise as possible. | Improvements in aerobic work capacity, muscle strength, and balance.
Recommendations are universal, but for individuals with illness, there may be special recommendations.
Medical advice may be required before exercise commences. Benefits of carrying out the activity are the same as for adults, and better functional health and independence. |
Compiled from FYSS 2017 ( www.fyss.se ) and WHO 2017 ( www.who.int ). 3. Aerobic and Muscle-Strengthening Physical ActivityPhysical activity is categorized according to FYSS as: (1) Aerobic physical activity and (2) muscle-strengthening physical activity. Physical activity in everyday life and exercise training is mainly an aerobic activity, where a majority of energy production occurs via oxygen-dependent pathways. Aerobic physical activity is the type of activity typically associated with stamina, fitness, and the biggest health benefits [ 29 , 30 , 31 ]. Muscle-strengthening physical activity is referred to in everyday language as “strength training” or “resistance training” and is a form of physical exercise/training that is primarily intended to maintain or improve various forms of muscle strength and increase or maintain muscle mass [ 32 ]. Sometimes, another category is defined: Muscle-enhancing physical activity, important for maintenance or improvement of coordination and balance, especially in the elderly [ 33 ]. According to these definitions, muscle-strengthening activities primarily involve the body’s anaerobic (without oxygen) energy systems, proportionally more as intensity increases. Exercise intensity can be expressed in absolute or relative terms. Absolute intensity means the physical work (for example; Watts [W], kg, or metabolic equivalent [MET]), while relative intensity is measured against the person’s maximum capacity or physiology (for example; percentage of maximum heart rate (%HR), rate of perceived exhaustion (RPE), W·kg −1 or relative oxygen uptake in L·min −1 ·kg −1 (VO 2 )). In terms of recommendations to the public, as in Table 1 , the intensity is often described in subjective terms (“makes you breathe harder” for moderate intensity, and “makes you puff and pant” for vigorous intensity) [ 27 ]. While objective criteria such as heart rate and accelerometry will capture the intensity of activity, they may not distinguish between different types of physical activity behaviors [ 34 ]. FYSS defines low intensity as 20%–39% of VO 2 max, <40 %HR, 1.5–2.9 METs; moderate intensity as 40%–59% of VO 2 max, 60–74 %HR, 3.0–5.9 METs, and vigorous intensity as 60%–89% of VO 2 max, 75–94 %HR, 6.0–8.9 METs. Absolute intensity, however, can vary greatly between individuals where a patient with heart disease may have a maximal capacity of <3 MET, and an elite athlete >20 MET [ 35 ]. 4. How does the Body Adapt to Physical Activity and Training?Adaption to physical activity and training is a complex physiological process, but may, in the context of this paper, be simplified by a fundamental basic principle:” The general adaptation syndrome (GAS)” [ 36 , 37 , 38 ]. This principle assumes that physical activity disturbs the body’s physiological balance, which the body then seeks to restore, all in a dose-related response relationship. The overload principle states that if exercise intensity is too low, overload is not reached to induce desired physiological adaptations, whereas an intensity too high will result in fatigue and possibly overtraining. Thus, for adaptation to occur, greater than normal stress must be induced, interspersed with sufficient recovery periods for restoration of physiological balance [ 39 ]. During and immediately after physical exercise/training, functions of affected tissues and systems are impaired, manifested as temporarily decreased performance. You feel tired. In order to gradually improve performance capacity, repeated cycles of adequate overload and recovery are required [ 40 ]. In practice, positive effects can be seen after a relatively short period of a few weeks, but more substantial improvements if the training is maintained for a longer period. As a rule of thumb, it is assumed that all people can adapt to physical activity and exercise, but the degree of adaptation depends on many factors, including age, heredity, the environment, and diet [ 41 , 42 , 43 , 44 ]. The hereditary factor (genetics) may be the most critical for adaptation [ 45 ]. The degree of adaptation also depends on how the person in question trained previously; a well-trained athlete usually does not have the same relative improvement as an untrained one. Even if training is thought to be specific to mode, intensity, and duration, there are some overlaps. For example, it has been found that strength training in some individuals contributes to a relatively large positive impact on health and endurance, effects previously associated primarily with aerobic exercise [ 46 , 47 ]. The overload principle may, if applied too vigorously in relation to a person’s individual adaptation ability, have detrimental effects, including reduced performance, injury, overtraining, and disease [ 10 ]. Training is a commodity that must be renewed; otherwise, you gradually lose achieved performance improvements [ 48 ], although some capacities, such as muscle memory, seem to persist for life [ 49 ]. General recommendations for health may be stated, but individual predispositions make general training schedules for specific performance effects unpredictable. All exercise training should be adjusted to individual purposes, goals, and circumstances. 5. Health Effects of Physical Activity and TrainingHuman biology requires a certain amount of physical activity to maintain good health and wellbeing. Biological adaption to life with less physical activity would take many generations. People living today have, more or less, the same requirements for physical activity as 40,000 years ago [ 50 , 51 ]. For an average man with a body weight of 70 kg, this corresponds to about 19 km daily walking in addition to everyday physical activity [ 52 ]. For most people, daily physical activity decreases, while planned, conscious exercise and training increases [ 19 , 53 ]. Unfortunately, average daily energy intake is increasing more than daily energy output, creating an energy surplus. This is one reason for the increasing number of overweight people, and a strong contributor to many health problems [ 54 ]. More sedentary living (not reaching recommended level of physical activity), combined with increased energy intake, impairs both physical and mental capabilities and increases the risk of disease. Despite this, Swedes (as an example) seemed to be as physically active and stressed but had better general health in 2015, compared to 2004 ( Figure 1 ). Compared to 2004–2007, the Swedish population in 2012–2015 reported better overall health (more county-dots are blue) and less fatigue (smaller county-dots) with similar level of physical activity (~65% indicated at least 30 min daily physical activity) and stress (~13% were stressed).  Selected physical and mental health indicators of a Sweden cohort, in relation to the degree of physical activity for the period of years 2004–2007 ( N = 29,254) and years 2012–2015 ( N = 38,553). Surveyed subjects are age 16 to 84 years old, with data representing median scores of four years, not normalized for age. Y-axis: Percentage of subjects reporting “stressed”; X-axis: Percentage of subjects indicating physical active at least 30 minutes each day. Each dot represents one County (Län), dot-size indicates self-reported fatigue, and color self-reported healthiness of the County. If 70% of the population states they are having “Good/Very good” health, the dot is blue. If less than 70% states they are having good/very good health, the dot is red. The circle indicated with a black arrow corresponds to nation median. The black line connected to the nation circle represents the movement in the X–Y plane from the year 2004 to 2007, and from 2012 to 2015, respectively. Data retrieved from the Public Health Agency of Sweden 2019-04-22 ( www.folkhalsomyndigheten.se ). Results in Figure 1 may in part be explained by a polarization of who is physically active: Some individuals are extremely active, others very inactive, giving a similar central tendency (mean/median). As physical activity and mental stress are not changed, but health is, the figure indicates that other factors must be more important to our overall health and fatigue. Recently, a national study of Swedish 11- to 15-year-olds concluded that this age group is inactive for most of their time awake, that is, sitting, standing or moving very little [ 55 ]. Time as inactive increased with age, from 67 percent for 11-year-olds to 75 percent for 15-year-olds. The study states that in all age groups, the inactive time is evenly distributed over the week, with school time, leisure time, and weekend. Further, those who feel school-related stress have more inactive time, both overall and during school hours, than those who have less school-related stress. People active in sports have, in general, better health than those who do not participate in sports, because they are physically and mentally prepared for the challenges of sports, abilities that in many cases can be transferred to other parts of life [ 56 ]. However, there is a certain bias in this statement. Sport practitioners are already positively selected, because sickness and injury may prevent participation. As many health benefits of sport are related to the level of physical activity, separation of sport and physical exercise may be problematic. Regardless, societal benefits of these health effects can be seen in lower morbidity, healthier elderly, and lower medical costs [ 7 , 57 , 58 ]. Health effects of physical activity in many cases follow a dose–response relationship; dose of physical activity is in proportion to the effect on health [ 59 , 60 ]. Figure 2 depicts the relationship between risk of death and level of physical activity, in a Finnish twin cohort, adjusted for smoking, occupational group, and alcohol consumption [ 59 ]. Odds ratio (OR) for the risk of all-cause mortality in a larger sample in the same study was 0.80 for occasional exercisers ( p = 0.002, 95% CI = 0.69–0.91). This dose–response relationship between risk of all-cause mortality and physical activity is evident in several extensive studies [ 60 , 61 , 62 ]. The total dose is determined by the intensity (how strenuous), duration (duration), and frequency (how often). While Figure 2 shows sex differences in death rates, it is likely that sedentary behavior is equally hazardous for men and women, but inconsistent results sometime occur due to inadequate assessment measures, or low statistical power [ 59 , 63 ]. To obtain the best possible development due to physical exercise/training, both for prevention and treatment purposes, a basic understanding of how these variables affect the dose of activity is required, as well as understanding how they can be modified to suit individual requirements. A physically active population is important for the health of both the individual and society, with sport participation being one, increasingly important, motivator for exercise.  Relative risk (odds ratio; OR) of premature death in relationship to level of physical activity, in 286 male and 148 female twin pairs, adjusted for smoking, occupational group, and use of alcohol [ 59 ]. There is strong scientific evidence supporting an association between physical exercise/training and good physical and mental health. For example: A reduction in musculoskeletal disorders and reduced disability due to chronic disease [ 27 , 64 ], better mental health with reduced anxiety [ 65 , 66 ], insomnia [ 67 ], depression [ 31 ], stress [ 68 ], and other psychological disorders [ 69 ]. Physical and mental health problems are related to an increased risk of developing a number of our major public health diseases and may contribute to premature death ( Table 2 ). Health-related physiological effects of aerobic and muscle strengthening physical activity. Green circle indicates that the activity contributes with an effect, whereas a red circle indicates that the activity has no proven effect. Orange circle indicates that the activity may in some cases be effective. | Effects on the Body | Health Effects | Aerobic | |
|---|
| Larger proportion slow-twitch fibers [ , ] | Lower risk for metabolic syndrome with increased exchange of gases and nutrition [ , ] | | | | Larger proportion slow-twitch [ ] | Increased strength, coordination and balance in elderly [ ] and in sickness [ ], lower risk for fall [ ] | | | | Formation of new capillaries [ ] | Increased aerobic capacity [ ] | | | | Improved endothelial function [ ] | Lower risk for cardiovascular disease [ ], improved function in heart disease [ ] | | | | Increased mitochondrial volume [ ] | Increased aerobic capacity [ ] | | | | Improved glucose transport [ ] | Lower risk or metabolic syndrome/Type-2 diabetes [ ] | | | | Improved insulin sensitivity [ ] | Improved health in people with Type-2 diabetes [ ], prevention of Typ-2 diabetes [ ] | | | | Increased heart capacity [ ] | Lower risk for cardiovascular disease [ ], fewer depressions [ , ], also in children [ ] | | | | Increased skeletal volume and mineral content [ ] | Improved skeletal health [ , ] | | | | Improved body composition [ ] | Lower risk for metabolic syndrome [ ] | | | | Improved blood pressure regulation [ , ] | Lower risk for cardiopulmonary disease [ ] | | | | Improved blood lipid profile [ ] | Lower risk for cardiopulmonary disease in elderly [ , ] and Alzheimer’s [ ]
No effect on blood lipid profiles in children and adolescents [ ] | | | | Improved peripheral nerve function [ ] | Better coordination, balance and reaction [ , ], especially in children and elderly [ ] | | | | Enhanced release of signaling substances [ , ] | Better sleep [ ], less anxiety [ ], treatment of depression [ ] | | | | Improved hippocampus function [ ] | Improved cognition and memory [ ], less medication [ ] | | | | Positive effects on mental capacity [ ] | Counteract brain degeneration by diseases [ ] and age [ ] | | | | Improved immune function [ ] | Decreased overall risk for disease [ , ], anti-inflammatory effects [ , ] | | | | Strengthening the connection between brain, metabolism and immune function [ ] | Decreased risk for disease [ ], improved metabolism [ ], decreased risk for depression [ ] | | | | Improved intestinal function [ , ] | Improved health [ ], mitigated metabolic syndrome, obesity, liver disease, and some cancers [ ] | | |
5.1. Effects on Physical HealthThe effects of physical activity and exercise are both acute (during and immediately after) and long-lasting. Effects remaining after a long period of regular physical activity have far-reaching consequences for health and are described below. For example, some muscle enzymes’ activity can be quickly increased by physical exercise/training but just as quickly be lost when idle [ 118 ]. Other changes remain for months or years even if training ends—for instance, increased number and size of muscle fibers and blood vessels [ 49 , 119 , 120 ]. Good health, therefore, requires physical activity to be performed with both progression and continuity. Most of the conducted physical exercise/training is a combination of both aerobic and muscle strengthening exercise, and it can be difficult to distinguish between their health effects ( Table 2 ). To describe ill-health, indicators of life expectancy, disease incidence (number), and prevalence (how often) are used [ 121 ]. In describing the relationship between physical activity and falling ill with certain diseases, the dose–response relationship, the effect size (the risk reduction that is shown in studies), and the recommended type and dose of physical activity are considered [ 122 ]. Table 3 shows the relative effects of regular physical activity ton the risk of various diseases (US Department of Human Services, 2009). The greatest health gains are for people who move from completely sedentary to moderately active lifestyles, with health effects seen before measurable improvements in physical performance. Previously, most scientific studies collected data only on aerobic physical activity. However, resistance exercise also shows promising health (mental and physical) and disease-prevention effects [ 123 , 124 , 125 , 126 , 127 ]. Disease prevention effects of regular physical activity. | Health Condition | Risk Reduction or Health Improvement | Recommendations for Physical Activity | Dose-Response Relationship | Differences between Sex, Age, Ethnicity etc. |
|---|
| | 30% (44% elderly) | General recommendations | Yes | No | | | 20%–35% | General recommendations | Yes | Insufficient evidence | | | 30%–40% | General recommendations | Yes | No | | | 25%–42% | General recommendations, data primarily on aerobic PA | Yes | Insufficient evidence | | | Brain cancer: Limited evidence ; Breast cancer: 20%; Bladder cancer: 13%–15%; Colon cancer: 30%; Endometrial cancer: 17%–35%;
Esophageal cancer : 6%–21%; Gastric cancer: 19%; Head & neck cancers: 15%–22%, limited evidence; Hematological cancers: No-low effect, limited evidence ; Lung cancer: 13%–26%; Ovarian cancer: Limited/conflicting evidence; Pancreatic & prostate cancer: Limited evidence; Renal cancer: 11%–23%; Rectal cancer: No risk reduction, limited evidence; Thyroid cancer: No risk reduction | General recommendations, data primarily on aerobic PA | Renal & thyroid cancer: No.
Lung, hematological, head and neck cancers: Limited evidence.
Other; Yes. | Breast cancer: Weaker evidence for Hispanic and Black women.
Gastric cancer: Weaker evidence for women
Renal cancer: Weaker evidence for Asians
Lung cancer: Greater effect for women
Other: Limited evidence/No known difference | | | PA alone, without diet intervention only has an effect at large volume | General recommendations, combined with diet interventions | Yes | No | | | PA supports weight maintenance | General recommendations, stronger evidence for aerobic PA | Limited evidence | Insufficient evidence | | | 36%–68% for hip fracture
1%–2% increased bone density | General recommendations including muscle- strengthening physical activity | Yes | Hip fracture: Largest effect in elderly women
Bone density: Largest effect in women | | | Magnitude is highly variable and mode-dependent | Weight bearing activity | Yes | Decreased effect with age | | | 30% increased chance to counteract or postpone a decrease in functional strength/capacity
30% lower risk of falls | General recommendations including muscle- and skeletal-strengthening physical activity | Functional health: Yes
Falls: No/unclear | Increased functional capacity mostly seen in older adults ages 65 or more. | | | 20%–30% lower | General recommendations | Yes | No | | | Improved quality, sleep onset latency and total sleep time | General recommendations | No | No | | | 20%–30% lower | General recommendations | No | No | | | 20%–30% lower | General recommendations | No | No | | | Improved for preadolescent children and adults aged 50 years or older | General recommendations | Conflicting findings | Insufficient evidence for adolescents and adults. Ethnicity: No. |
Compiled from US Department of Health and Human Service, https://health.gov/paguidelines/report/ [ 62 , 146 ] 1 : Risk reduction refers to the relative risk in physically active samples in comparison to a non-active sample, i.e., a risk reduction of 20% means that the physically active sample has a relative risk of 0.8, compared to the non-active sample, which has 1.0. 2 : In general, general recommendations for PA that are described and referred to herein apply to most conditions. However, in some cases, more specific recommendations exist, more in depth described by the US Department of Health and Human Service, amongst others [ 62 ]. 3 : Evidence is dependent on cancer subtype; refer to US Department of Health and Human Service [ 62 ] for in-depth guidance. PA = Physical. Aerobic physical activity has been shown to benefit weight maintenance after prior weight loss, reduce the risk of metabolic syndrome, normalize blood lipids, and help with cancer/cancer-related side effects ( Table 2 and Table 3 ), while effects on chronic pain are not as clear [ 29 ]. Muscle-strengthening physical activity has, in contrast to aerobic exercise, been shown to reduce muscle atrophy [ 128 ], risk of falling [ 75 ], and osteoporosis [ 74 ] in the elderly. Among the elderly, both men and women adapt positively to strength training [ 129 ]. Strength training also prevents obesity [ 130 ], enhances cognitive performance if done alongside aerobic exercise [ 131 ], counteracts the development of neurodegenerative diseases [ 132 , 133 , 134 ], reduces the risk of metabolic syndrome [ 135 ], counteracts cancer/cancer-related side effects [ 135 , 136 ], reduces pain and disability in joint diseases [ 137 ], and enhances bone density [ 137 , 138 ]. The risk of falling increases markedly with age and is partly a result of reduced muscle mass, and reduced coordination and balance [ 76 , 139 , 140 ]. A strong correlation between physical performance, reduced risk of falls, and enhanced quality of life is therefore, not surprisingly, found in older people [ 141 ]. Deterioration in muscle strength, but not muscle mass, increases the risk of premature death [ 142 ] but can be counteracted by exercise as a dose–response relationship describes the strength improvement in the elderly [ 122 , 143 ]. Recommendations state high-intensity strength training (6–8 repetitions at 80% of 1-repetition maximum) as most effective [ 144 ]. Muscle strengthening physical activity for better health is recommended as a complement to aerobic physical activity [ 29 ]. Amongst the elderly, vibration training can be an alternative to increase strength [ 145 ]. 5.2. Effects on Mental HealthMental illness is a global problem affecting millions of people worldwide [ 147 ]. Headache, stress, insomnia, fatigue, and anxiety are all measures of mental ill health. The term “ ill health ” constitutes a collection of several mental health problems and symptoms with various levels of seriousness. Studies have compared expected health benefits from regular physical activity for improvement of mental health with other treatments, for example, medication. Most recent studies show that physical activity and exercise used as a primary, or secondary, processing method have significant positive effects in preventing or alleviating depressive symptoms [ 31 , 148 , 149 , 150 , 151 ] and have an antidepressant effect in people with neurological diseases [ 152 ]. Training and exercise improve the quality of life and coping with stress and strengthen self-esteem and social skills [ 69 , 153 ]. Training and exercise also lessen anxiety in people who are diagnosed with an anxiety- or stress-related disease [ 68 ], improve vocabulary learning [ 154 ], memory [ 155 , 156 ], and creative thinking [ 157 ]. The same Swedish data as used in Figure 1 show that between the years 2004–2007 and 2012–2015 anxiety, worry, and insomnia decreased but were not obviously correlated to the slightly increased level of physical activity in the population during the same period. Thus, in a multifactorial context, the importance of physical exercise alone cannot be demonstrated in this dataset. Some of the suggested physiological explanations for improved mental health with physical activity and exercise are greater perfusion and increased brain volume [ 107 , 158 ], increased volume of the hippocampus [ 106 ], and the anti-inflammatory effects of physical activity, reducing brain inflammation in neurological diseases [ 159 ]. Physical exercise may also mediate resilience to stress-induced depression via skeletal muscle peroxisome proliferator-activated receptor gamma coactivator 1-alpha (PGC-1α), enhancing kynurenine conversion to kynurenine acid, which in turn protects the brain and reduces the risk for stress-induced depression [ 153 ]. Further, increased release of growth factors, endorphins, and signaling molecules are other exercise-induced enhancers of mental health [ 69 ]. 6. How Sport Affects HealthSport’s main purposes are to promote physical activity and improve motor skills for health and performance and psychosocial development [ 56 ]. Participants also gain a chance to be part of a community, develop new social circles, and create social norms and attitudes. In healthy individuals, and patients with mental illness, sport participation has been shown to provide individuals with a sense of meaning, identity, and belonging [ 160 , 161 ]. Whether the sport movement exists or not, training and competition including physical activity will happen. Sport’s added values, in addition to the health benefits of physical activity, are therefore of interest. Some argue that it is doubtful, or at least not confirmed, that health development can come from sport, while others believe that healthy sport is something other than health, reviewed in depth by Coakley [ 162 ]. In a sporting context, health is defined as subjective (e.g., one feels good), biological (e.g., not being sick), functional (e.g., to perform), and social (e.g., to collaborate) [ 163 ]. Holt [ 56 ] argued that the environment for positive development in young people is distinctly different from an environment for performance, as the latter is based on being measured and assessed. That said, certain skills (goal setting, leadership, etc.) can be transferred from a sporting environment to other areas of life. The best way to transfer these abilities is, at the moment, unclear. Having the goal to win at all costs can be detrimental to health. This is especially true for children and adolescents, as early engagement in elite sports increases the risk of injury, promotes one-dimensional functional development, leads to overtraining, creates distorted social norms, risks psychosocial disorders, and has the risk of physical and psychological abuse [ 15 , 164 ]. Of great importance, therefore, is sport’s goal of healthy performance development, starting at an early age. For older people, a strong motivating factor to conduct physical activity is sports club membership [ 165 ]. One can summarize these findings by stating sport’s utility at the transition between different stages of the life; from youth to adulthood and from adulthood to old age. There, sports can be a resource for good physical and mental health [ 166 ]. Today, a higher proportion of the population, compared to 50 years ago, is engaged in organized sports, and to a lesser extent performs spontaneous sports ( Figure 3 ), something that Engström showed in 2004 [ 17 ] and is confirmed by data from The Swedish Sports Confederation ( www.rf.se ). Of the surveyed individuals in 2001, 50%–60% of children and young people said they were active in a sports club. The trend has continued showing similar progression to 2011, with up to 70% of school students playing sports in a club. Furthermore, the study shows that those active in sport clubs also spontaneously do more sports [ 167 ]. Similar data from the years 2007–2018, compiled from open sources at The Swedish Sports Confederation, confirm the trend with an even higher share of youths participating in organized sports, compared to 1968 and 2001 ( Figure 4 ).  Spontaneous sport has decreased over the last decades, to the advantage of organized sport. Data compiled from Engström, 2004, The Swedish Research Council for Sport Science.  Data compiled from open sources report Sport Statistics (Idrotten i siffror) at The Swedish Sports Confederation for the year 2011 ( www.rf.se ). Taking part in sports can be an important motivator for physical activity for older people [ 165 , 166 ]. With aging, both participation in sports ( Figure 4 ) and physical activity in everyday life [ 168 ] decreases. At the same time, the number of people who are physically active both in leisure and in organized sports increases (The Public Health Agency of Sweden 2017; www.folkhalsomyndigheten.se ). Consequently, among elderly people, a greater proportion of the physical activity occurs within the context of sport [ 8 , 28 ]. Together, research shows that organized sports, in clubs or companies, are more important for people’s overall physical activity than ever before. Groups that are usually less physically active can be motivated through sport—for example, elderly men in sport supporters’ clubs [ 169 ], people in rural areas [ 170 ], migrants [ 171 ], and people with alternative physical and mental functions [ 172 ]. No matter how you get your sporting interest, it is important to establish a physical foundation at an early age to live in good health when you get older ( Figure 5 ). As seen in Figure 5 , a greater sport habitus at age 15 results in higher physical activity at 53 years of age. Early training and exposure to various forms of sports are therefore of great importance. Participation creates an identity, setting the stage for a high degree of physical activity later in life [ 173 ].  Odds ratio (OR) of physical activity at age 53 in relation to Sport habitus at age 15. Sport habitus (“the total physical capital"), including cultural capital, athletic diversity, and grades in physical education and health are, according to Engström [ 173 ], the factors most important for being physically active in later life. For a further discussion on sport habitus, the readers are referred to Engström, 2008 [ 173 ]. Numbers above bar show the 95% confidence interval. ** = significant difference from “Very low”, p < 0.01. *** = p < 0.001. 7. Sport’s Effects on the Health of Children and Young PeopleThe effects of participation in organized sports for children and young people are directly linked to physical activity, with long term secondary effects; an active lifestyle at a young age fosters a more active lifestyle as an adult. As many diseases that are positively affected by physical activity/exercise appear later in life, continued participation in sport as an adult will reduce morbidity and mortality. It must be emphasized that good physical and mental health of children and young people participating in sport requires knowledge and organization based on everyone’s participation. Early specialization counteracts, in all regards, both health and performance development [ 174 , 175 ]. 7.1. Positive AspectsAccording to several reviews, there is a correlation between high daily physical activity in children and a low risk for obesity, improved development of motor and cognitive skills, as well as a stronger skeleton [ 176 , 177 ]. Positive effects on lipidemia, blood pressure, oxygen consumption, body composition, metabolic syndrome, bone density and depression, increased muscle strength, and reduced damage to the skeleton and muscles are also described [ 178 , 179 ]. If many aspects are merged in a multidimensional analysis [ 8 , 173 ], the factors important for future good health are shown to be training in sports, broad exposure to different sports, high school grades, cultural capital, and that one takes part in sport throughout childhood ( Table 4 ). Compiled health profiles for men and women at the age of 20 years, depending on participation in organized sports at the age of 5, 7, 8, 10, 14, and 17 years. | Physical Activity at Age 20 Years | Girls | Boys |
|---|
| Sport Participation as Young |
|---|
| Participate | Quit | Never | Participate | Quit | Began late |
|---|
| | ⮉ | ⮉ | ⮋ | ⮉ | ⮉ | ⮋ | | | ⇔ | ⇔ | ⇔ | ⮉ | ⮉ | ⮋ | | | ⇔ | ⇔ | ⇔ | ⇔ | ⇔ | ⇔ | | | ⇔ | ⇔ | ⇔ | ⇔ | ⇔ | ⇔ | | | ⇔ | ⇔ | ⇔ | ⮋ | ⮉ | ⮉ | | | ⮉ | ⮉ | ⮋ | ⮉ | ⮋ | ⮉ | | ) | ⮉ | ⮉ | ⮋ | ⮉ | ⮋ | ⮉ | | | ⮉ | ⮉ | ⮋ | ⇔ | ⇔ | ⇔ | | | ⇔ | ⇔ | ⇔ | ⇔ | ⇔ | ⇔ | | | ⇔ | ⇔ | ⇔ | ⇔ | ⮉ | ⇔ | | | ⇔ | ⇔ | ⇔ | ⇔ | ⇔ | ⇔ | | | ⇔ | ⇔ | ⇔ | ⇔ | ⇔ | ⇔ |
Classification with repeated latent class analysis creates three groups for girls and boys, respectively: Children who never participated (girls only), participated, quit prematurely, or began late (only boys) in sports. Arrows indicate whether participation in sports at young age has an effect on health at 20 years of age. Green up arrow is positive, red down arrow negative, and a horizontal black double arrow shows that sport had no significant effect. Modified from Howie et. al., 2016 [ 8 ]. Psychological benefits of sports participation of young people were compiled by Eime et al. [ 1 ], where the conclusion was that sporting children have better self-esteem, less depression, and better overall psychosocial health. One problem with most of these studies, though, is that they are cross-sectional studies, which means that no cause–effect relationship can be determined. As there is a bias for participating children towards coming from socially secure environments, the results may be somewhat skewed. 7.2. Negative AspectsAs Table 4 and Table 5 show, there are both positive and negative aspects of sports. Within children’s and youth sports, early specialization to a specific sport is a common phenomenon [ 175 ]. There is no scientific evidence that early specialization would have positive impact, neither for health nor for performance later in life [ 175 ]. No model or method including performance at a young age can predict elite performance as an adult. By contrast, specialization and competitiveness can lead to injury, overtraining, increased psychological stress, and reduced training motivation, just to mention a few amongst many negative aspects [ 174 , 175 ]. Another important aspect is that those who are excluded from sports feel mentally worse [ 8 ]. As there is a relationship between depressive episodes in adolescence, and depression as adults [ 116 ], early exclusion has far-reaching consequences. Therefore, sports for children and young people have future health benefits by reducing the risk of developing depression and depressive symptoms, as well as improved wellbeing throughout life. Positive and negative aspects with sport (at young age). | Aspect | Positive | Negative |
|---|
| | Better self-esteem
Better academic results
That endurance and hard work pay off
Independence and responsibility
Making wise decisions
Keep a positive attitude
Manage stress
Set clear goals
Higher assessment of skills
Higher working standards
Better discipline
Late alcohol store
Lower alcohol consumption (in most sports)
Less drugs
Greater social capital
Better relationships with adults
Uses TV/PC less
Lower risk of school dropout | Emotional fatigue
One-dimensional identity
Risk of abuse
Increased stress
Injuries
Temptation for doping
Fear of punishment
Fear of failure
Feeling pressure from the surroundings
Fear of disappointing surroundings
Risk of burnout
Risk of overtraining
Poor sleep
Decrepit
Repeated infections
Risk of self-sacrifice
Risk of self-injury
Increased risk of destructive decisions (doping, cheating etc.)
Risk of depression in case of rejection | | | The usefulness of teamwork
Good communication
Larger contributions to society later in life
Larger contributions to the family later in life
Lower crime
Opportunity in developing countries
Increased chance of being active in sports clubs as older
Easier to reach with education | Less integrated with the family
Social isolation from other society | | | Greater physical literacy
Abilities to live a healthy life as adult and elderly
Less smoking
Less drugs
Lower body fat
Larger muscle mass
Beneficial metabolism
Higher aerobic and anaerobic capacity
Lower risk for fractures as older
Reduced general disease risk | Physical fatigue
Increased injury risk
Risk of eating disorders
Overtraining
Temptation for doping
Risk of abuse (physical and mental)
Unilateral training and development
For Para athletes, injury can be a double handicap
Worse oral health |
While some degree of sport specialization is necessary to develop elite-level athletes, research shows clear adverse health effects of early specialization and talent selection [ 180 ]. More children born during the fall and winter (September–December) are excluded [ 181 ], and as a group, they are less physically active than spring (January–April) children, both in sports and leisure ( Figure 6 ). In most sports and in most countries, there is a skewed distribution of participants when sorted by birth-date, and there are more spring children than fall children among those who are involved in sport [ 182 , 183 , 184 , 185 , 186 ]. Because a large part of the physical activity takes place in an organized form, this leads to lower levels of physical activity for late-born persons (Malm, Jakobsson, and Julin, unpublished data). Early orientation and training in physical activity and exercise will determine how active you are later in life. Greater attention must be given to stimulating as many children and young people as possible to participate in sport as long as possible, both in school and on their leisure time. According to statistics from the Swedish Sports Confederation in 2016, this relative-age effect persists throughout life, despite more starting than ending with sport each year [ 18 ].  The figure shows the distribution of 7597 children aged 10 years and younger who in 2014 were registered as active in one particular, individual sport in Sweden (data compiled from the Swedish Sport Confederation, www.rf.se ). Spring, Summer, and Fall represent January–April, May–August, and September–December, respectively. When summarize, the positive and negative aspects of sport at a young age can be divided into three categories: (1) Personal identification, (2) social competence, and (3) physiological capacity, briefly summarized in Table 5 . A comprehensive analysis of what is now popularly known as “physical literacy” has recently been published [ 187 ]. 7.3. Relevance of SportsSports can make children and young people develop both physically and mentally and contribute with health benefits if planned and executed exercise/training considers the person’s own capacities, social situation, and biological as well as psychological maturation. In children and adolescents, it is especially important to prevent sports-related injuries and health problems, as a number of these problems are likely to remain long into adulthood, sometimes for life. Comprehensive training is recommended, which does not necessarily mean that you have to participate in various sports. What is required is diverse training within every sport and club. Research shows that participation in various sports simultaneously during childhood and adolescence is most favorable for healthy and lifelong participation [ 8 , 173 , 188 , 189 ]. 8. Sport’s Effects on the Health of Adults and the ElderlyAdults who stop participating in sports reduce their physical activity and have health risks equal to people who have neither done sports nor been physical [ 190 , 191 ]. Lack of adherence to exercise programs is a significant hindrance in achieving health goals and general physical activity recommendations in adults and the elderly [ 192 ]. While several socioeconomic factors are related to exercise adherence, it is imperative that trainers and health care providers are informed about factors that can be modulated, such as intervention intensity (not to high), duration (not too long), and supervision, important for higher adherence, addressed more in depth by Rivera-Torres, Fahey and Rivera [ 192 ]. Healthy aging is dependent on many factors, such as the absence of disease, good physical and mental health, and social commitment (especially through team sports or group activities) [ 193 ]. Increased morbidity with age may be partly linked to decreased physical activity. Thus, remaining or becoming active later in life is strongly associated with healthy aging [ 194 ]. With increased age, there is less involvement in training and competition ( Figure 4 ), and only 20% of adults in Sweden are active, at least to some extent, in sports clubs, and the largest proportion of adults who exercise do it on their own. The following sections describes effects beyond what is already provided for children and youths. 8.1. Positive AspectsParticipation in sports, with or without competition, promotes healthy behavior and a better quality of life [ 166 ]. Exclusion from sports at a young age appears to have long-term consequences, as the previously described relative age effect ( Figure 6 ) remains even for master athletes (Malm, Jakobsson, and Julin, unpublished data). Because master athletes show better health than their peers [ 95 ], actions should be taken to include adults and elderly individuals who earlier in life were excluded from, or never started with sport [ 195 ]. As we age, physical activity at a health-enhancing intensity is not enough to maintain all functions. Higher intensity is required, best comprising competition-oriented training [ 196 , 197 ]. One should not assume that high-intensity exercise cannot be initiated by the elderly [ 198 ]. Competitive sports, or training like a competitive athlete as an adult, can be one important factor to counter the loss of physical ability with aging [ 199 ]. In this context, golf can be one example of a safe form of exercise with high adherence for older adults and the elderly, resulting in increased aerobic performance, metabolic function, and trunk strength [ 200 , 201 ]. 8.2. Negative AspectsIncreased morbidity (e.g., cardiovascular disease) with aging is seen also among older athletes [ 202 ] and is associated with the same risk factors as in the general population [ 203 ]. An increased risk of cardiovascular disease among adults (master) compared to other populations has been found [ 204 ]. Unfortunately, the designs and interpretations of these studies have been criticized, and the incidence of cardiac arrest in older athletes is unclear [ 205 ]. In this context, the difference between competitive sports aiming to optimize performance and recreational sports has to be taken into account, where the former is more likely to induce negative effects due to high training loads and/or impacts during training and games. Although high-intensity training even for older athletes is positive for aerobic performance, it does not prevent the loss of motor units [ 206 ]. Quality of life is higher in sporting adults compared to those who do not play sports, but so is the risk of injury. When hit by injury, adults and young alike may suffer from psychological disorders such as depression [ 207 ], but with a longer recovery time in older individuals [ 208 ]. As with young athletes, secession of training at age 50 years and above reduces blood flow in the brain, including the hippocampus, possibly related to long-term decline in mental capacity [ 209 ]. 8.3. Relevance of SportAs for children and young people, many positive health aspects come through sport also for adults and the elderly [ 210 ]. Sport builds bridges between generations, a potential but not elucidated drive for adults’ motivation for physical activity. The percentage of adults participating in competitive sports has increased in Sweden since 2010, from about 20 percent to 30 percent of all of those who are physically active [ 18 ], a trend that most likely provides better health for the group in the 30–40 age group and generations to come. 9. Recommendations for Healthy Sport- 1. Plan exercise, rest, and social life. For health-promoting and healthy-aging physical activity, refer to general guidelines summarized in this paper: Aerobic exercise three times a week, muscle-strengthening exercise 2–3 times a week.
- 2. Set long-term goals.
- 3. Adopt a holistic performance development including physiological, medical, mental, and psychosocial aspects.
- ○ a. Exercise load (time, intensity, volume);
- ○ b. Recovery (sleep, resting heart rate, appetite, estimated fatigue, etc.);
- ○ c. Sickness (when–where–how, type of infections, how long one is ill, etc.);
- ○ d. Repeat type- and age-specific physical tests with relevant evaluation and feedback;
- ○ e. Frequency of injuries and causes.
- ○ a. Motivation for training, competition, and socializing;
- ○ b. Personal perception of stress, anxiety, depression, alienation, and self-belief;
- ○ c. Repeat type- and age-specific psychological tests with relevant evaluation and feedback.
- 6. Register and interpret signs of overtraining, such as reduced performance over time, while maintaining or increasing exercise load.
Author ContributionsC.M. and A.J. conceived and designed the review. C.M., A.J., J.J. and interpreted the data and drafted the manuscript. J.J. edited the manuscript, tables, and figures. All authors approved the final version. This work was supported by the Swedish Sports Confederation. Conflicts of InterestThe authors declare no conflict of interest.  Academia.edu no longer supports Internet Explorer. To browse Academia.edu and the wider internet faster and more securely, please take a few seconds to upgrade your browser . - We're Hiring!
- Help Center
Sports Medicine- Most Cited Papers
- Most Downloaded Papers
- Newest Papers
- Last »
- Exercise Physiology Follow Following
- Aquatic Sports Follow Following
- Sport Science Follow Following
- Bioenergetics Follow Following
- Hypoxia Follow Following
- Triathlon Follow Following
- Altitude Follow Following
- Swimming Follow Following
- Sport Biomechanics Follow Following
- Sports Performance Follow Following
Enter the email address you signed up with and we'll email you a reset link. - Academia.edu Journals
- We're Hiring!
- Help Center
- Find new research papers in:
- Health Sciences
- Earth Sciences
- Cognitive Science
- Mathematics
- Computer Science
- Academia ©2024
Cannabinoid Therapy in Athletics: A Review of Current Cannabis Research to Evaluate Potential Real-World Cannabinoid Applications in Sport- Review Article
- Published: 21 August 2024
Cite this article - Elizabeth S. Thompson ORCID: orcid.org/0009-0007-1159-0375 1 ,
- Jane Alcorn ORCID: orcid.org/0000-0002-3473-2635 1 &
- J. Patrick Neary ORCID: orcid.org/0000-0003-2480-8031 2
69 Accesses 28 Altmetric Explore all metrics The increasing legalization of Cannabis sativa plant products has sparked growing interest in their therapeutic applications. Prohibition laws established in 1937 hindered formal research on cannabis, a plant with cultural and medicinal roots dating back to 2700 BC in Chinese history. Despite regulatory hurdles, published research on cannabis has emerged; yet elite athletes remain an underrepresented population in these studies. Athletes, known for exploring diverse substances to optimize performance, are drawn to the potential benefits of cannabinoid therapy, with anecdotal reports suggesting positive effects on issues ranging from anxiety to brain injuries. This review aims to evaluate empirical published cannabis research with a specific focus on its potential applications in athletics. The changing legal landscape, especially the removal of cannabis from drug testing programs in leagues such as the National Basketball Association (NBA), and endorsements by Major League Baseball (MLB) for cannabinoid products and the National Football League (NFL) for cannabis research, reflects a shift in the acceptability of such substances in sports. However, stigma, confusion, and a lack of education persist, hindering a cohesive understanding among sports organizations, including business professionals, policymakers, coaches, and medical/training staff, in addition to athletes themselves. Adding to the confusion is the lack of consistency with cannabinoid regulations from sport to sport, within or out of competition, and with cannabis bioactive compounds. The need for this review is underscored by the evolving attitudes toward cannabinoids in professional sports and the potential therapeutic benefits or harms they may offer. By synthesizing current cannabis research, this review aims to provide a comprehensive understanding of the applications and implications of cannabinoid use in the realm of athletics. This is a preview of subscription content, log in via an institution to check access. Access this articleSubscribe and save. - Get 10 units per month
- Download Article/Chapter or eBook
- 1 Unit = 1 Article or 1 Chapter
- Cancel anytime
Price includes VAT (Russian Federation) Instant access to the full article PDF. Rent this article via DeepDyve Institutional subscriptions  Similar content being viewed by others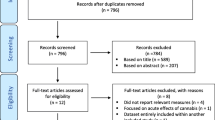 Chronic cannabis consumption and physical exercise performance in healthy adults: a systematic review Cannabidiol and Sports Performance: a Narrative Review of Relevant Evidence and Recommendations for Future ResearchCannabis and athletic performance. Pain S. A potted history. Nature. 2015;525(7570):Art. no. 570. https://doi.org/10.1038/525S10a . Article CAS Google Scholar Knox D. Why Charlotte’s web partnered with major league baseball to educate the world about CBD. Forbes. [Online]. Available: https://www.forbes.com/sites/daveknox/2023/03/14/why-charlottes-web-partnered-with-major-league-baseball-to-educate-the-world-about-cbd/ . Accessed 13 Sep 2023. NFL Awards $1 Million to Study Impact of Cannabis and CBD on Pain Management. NFL.com. [Online]. Available: https://www.nfl.com/playerhealthandsafety/health-and-wellness/pain-management/nfl-awards-1-million-to-study-impact-of-cannabis-and-cbd-on-pain-management . Accessed 13 Sep 2023. Vorkunov SCM. NBA and players association reach tentative agreement. The Athletic. [Online]. Available: https://theathletic.com/4370686/2023/04/01/new-nba-cba-agreement/ . Accessed 13 Sep 2023. Is the NHL the future of marijuana in pro sports? Why it could be. ESPN.com. [Online]. Available: https://www.espn.com/nhl/story/_/id/26046596/is-nhl-future-marijuana-pro-sports-why-be . Accessed 27 May 2024. Ziemianski D, Capler R, Tekanoff R, Lacasse A, Luconi F, Ware MA. Cannabis in medicine: a national educational needs assessment among Canadian physicians. BMC Med Educ. 2015;15(1):52. https://doi.org/10.1186/s12909-015-0335-0 . Article PubMed PubMed Central Google Scholar Balneaves LG, Alraja A, Ziemianski D, McCuaig F, Ware M. A national needs assessment of canadian nurse practitioners regarding cannabis for therapeutic purposes. Cannabis Cannabinoid Res. 2018;3(1):66–73. https://doi.org/10.1089/can.2018.0002 . St. Pierre M, Matthews L, Walsh Z. Cannabis education needs assessment among Canadian physicians-in-training. Complement Therap Med. 2020;49:102328. https://doi.org/10.1016/j.ctim.2020.102328 . Article Google Scholar Ewell TR, et al. Pharmacokinetic investigation of commercially available edible marijuana products in humans: potential influence of body composition and influence on glucose control. Pharmaceuticals (Basel). 2021;14(8):817. https://doi.org/10.3390/ph14080817 . Article CAS PubMed Google Scholar Hanuš LO, Meyer SM, Muñoz E, Taglialatela-Scafati O, Appendino G. Phytocannabinoids: a unified critical inventory. Nat Prod Rep. 2016;33(12):1357–92. https://doi.org/10.1039/C6NP00074F . Article PubMed Google Scholar Blatt-Janmaat K, Qu Y. The biochemistry of phytocannabinoids and metabolic engineering of their production in heterologous systems. Int J Mol Sci. 2021;22(5):Art. no. 5. https://doi.org/10.3390/ijms22052454 . Veilleux A, Di Marzo V, Silvestri C. The expanded endocannabinoid system/endocannabinoidome as a potential target for treating diabetes mellitus. Curr Diab Rep. 2019;19(11):117. https://doi.org/10.1007/s11892-019-1248-9 . “Cannabis (Marijuana) and Cannabinoids: What You Need To Know,” NCCIH. [Online]. Available: https://www.nccih.nih.gov/health/cannabis-marijuana-and-cannabinoids-what-you-need-to-know . Accessed 10 Jul 2024. Kruger DJ, Mokbel MA, Clauw DJ, Boehnke KF. Assessing health care providers’ knowledge of medical cannabis. Cannabis Cannabinoid Res. 2022;7(4):501–7. https://doi.org/10.1089/can.2021.0032 . Di Marzo V, Piscitelli F. The endocannabinoid system and its modulation by phytocannabinoids. Neurotherapeutics. 2015;12(4):692–8. https://doi.org/10.1007/s13311-015-0374-6 . Article CAS PubMed PubMed Central Google Scholar Di Marzo V. The endocannabinoidome as a substrate for noneuphoric phytocannabinoid action and gut microbiome dysfunction in neuropsychiatric disorders. Dialogues Clin Neurosci. 2020;22(3):259–69. https://doi.org/10.31887/DCNS.2020.22.3/vdimarzo . Sulcova A. Pharmacodynamics of cannabinoids. Arch Pharm Pharma Sci. 2019;3(1):011–8. https://doi.org/10.29328/journal.apps.1001013 . Cerqueira É, Marinho DA, Neiva HP, Lourenço O. Inflammatory effects of high and moderate intensity exercise—a systematic review. Front Physiol. 2020;10:1550. https://doi.org/10.3389/fphys.2019.01550 . Maayah ZH, Takahara S, Ferdaoussi M, Dyck JRB. The molecular mechanisms that underpin the biological benefits of full-spectrum cannabis extract in the treatment of neuropathic pain and inflammation. Biochim Biophys Acta (BBA) Mol Basis Dis. 2020;1866(7):165771. https://doi.org/10.1016/j.bbadis.2020.165771 . Ji Y, et al. Inflammation: Roles in Skeletal Muscle Atrophy. Antioxidants (Basel). 2022;11(9):1686. https://doi.org/10.3390/antiox11091686 . Fioranelli M, Roccia MG, Flavin D, Cota L. Regulation of inflammatory reaction in health and disease. Int J Mol Sci. 2021;22(10):Art. no. 10. https://doi.org/10.3390/ijms22105277 . Owens DJ, Twist C, Cobley JN, Howatson G, Close GL. Exercise-induced muscle damage: What is it, what causes it and what are the nutritional solutions? Eur J Sport Sci. 2019;19(1):71–85. https://doi.org/10.1080/17461391.2018.1505957 . Ditmer M, Gabryelska A, Turkiewicz S, Białasiewicz P, Małecka-Wojciesko E, Sochal M. Sleep problems in chronic inflammatory diseases: prevalence, treatment, and new perspectives: a narrative review. J Clin Med. 2021;11(1):67. https://doi.org/10.3390/jcm11010067 . Lacourt TE, Vichaya EG, Chiu GS, Dantzer R, Heijnen CJ. The high costs of low-grade inflammation: persistent fatigue as a consequence of reduced cellular-energy availability and non-adaptive energy expenditure. Front Behav Neurosci. 2018;12:78. https://doi.org/10.3389/fnbeh.2018.00078 . Karshikoff B, Sundelin T, Lasselin J. Role of inflammation in human fatigue: relevance of multidimensional assessments and potential neuronal mechanisms. Front Immunol. 2017;8:21. https://doi.org/10.3389/fimmu.2017.00021 . Chen L, et al. Inflammatory responses and inflammation-associated diseases in organs. Oncotarget. 2017;9(6):7204–18. https://doi.org/10.18632/oncotarget.23208 . Holzer-Geissler JCJ, et al. The Impact of Prolonged Inflammation on Wound Healing. Biomedicines. 2022;10(4):4. https://doi.org/10.3390/biomedicines10040856 . Bie B, Wu J, Foss JF, Naguib M. An overview of the cannabinoid type 2 receptor system and its therapeutic potential. Curr Opin Anaesthesiol. 2018;31(4):407–14. https://doi.org/10.1097/ACO.0000000000000616 . Cabral GA, Griffin-Thomas L. Emerging role of the cannabinoid receptor CB2 in immune regulation: therapeutic prospects for neuroinflammation. Expert Rev Mol Med. 2009;11: e3. https://doi.org/10.1017/S1462399409000957 . Osafo N, Yeboah OK, Antwi AO. Endocannabinoid system and its modulation of brain, gut, joint and skin inflammation. Mol Biol Rep. 2021;48(4):3665–80. https://doi.org/10.1007/s11033-021-06366-1 . Shahbazi F, Grandi V, Banerjee A, Trant JF. Cannabinoids and cannabinoid receptors: the story so far. iScience. 2020;23(7):101301. https://doi.org/10.1016/j.isci.2020.101301 . Zou S, Kumar U. Cannabinoid receptors and the endocannabinoid system: signaling and function in the central nervous system. Int J Mol Sci. 2018;19(3):Art. no. 3. https://doi.org/10.3390/ijms19030833 . Ahmed I, et al. Therapeutic attributes of endocannabinoid system against neuro-inflammatory autoimmune disorders. Molecules. 2021;26(11):Art. No. 11. https://doi.org/10.3390/molecules26113389 . Ajrawat P, et al. Medical cannabis use and inflammatory cytokines and chemokines among adult chronic pain patients. Cannabis Cannabinoid Res. 2024;9(1):267–81. https://doi.org/10.1089/can.2022.0143 . Fernández-Ruiz J. The biomedical challenge of neurodegenerative disorders: an opportunity for cannabinoid-based therapies to improve on the poor current therapeutic outcomes: Cannabinoids and neuroprotection. Br J Pharmacol. 2019;176(10):1370–83. https://doi.org/10.1111/bph.14382 . Khosropoor S, Alavi MS, Etemad L, Roohbakhsh A. Cannabidiol goes nuclear: the role of PPARγ. Phytomedicine. 2023;114: 154771. https://doi.org/10.1016/j.phymed.2023.154771 . Silvestri C, Di Marzo V. The gut microbiome-endocannabinoidome axis: a new way of controlling metabolism, inflammation, and behavior. Function. 2023;4(2):zqad003. https://doi.org/10.1093/function/zqad003 . Chan JZ, Duncan RE. Regulatory effects of cannabidiol on mitochondrial functions: a review. Cells. 2021;10(5):1251. https://doi.org/10.3390/cells10051251 . Castillo-Arellano J, Canseco-Alba A, Cutler SJ, León F. The polypharmacological effects of cannabidiol. Molecules. 2023;28(7):Art. No. 7. https://doi.org/10.3390/molecules28073271 . Martini S, Gemma A, Ferrari M, Cosentino M, Marino F. Effects of cannabidiol on innate immunity: experimental evidence and clinical relevance. Int J Mol Sci. 2023;24(4):Art. no. 4. https://doi.org/10.3390/ijms24043125 . Fernández-Ruiz J, et al. Cannabidiol for neurodegenerative disorders: important new clinical applications for this phytocannabinoid?: Cannabidiol and neurodegenerative disorders. Br J Clin Pharmacol. 2013;75(2):323–33. https://doi.org/10.1111/j.1365-2125.2012.04341.x . Reid M. A qualitative review of cannabis stigmas at the twilight of prohibition. J Cannabis Res. 2020;2(1):46. https://doi.org/10.1186/s42238-020-00056-8 . Clobes TA, Palmier LA, Gagnon M, Klaiman C, Arellano M. The impact of education on attitudes toward medical cannabis. PEC Innov. 2021;1: 100009. https://doi.org/10.1016/j.pecinn.2021.100009 . Turner SE, Williams CM, Iversen L, Whalley BJ. Molecular Pharmacology of Phytocannabinoids. In: Kinghorn AD, Falk H, Gibbons S, Kobayashi J, editors. Phytocannabinoids, progress in the chemistry of organic natural products, vol. 103. Cham: Springer International Publishing; 2017. p. 61–101. https://doi.org/10.1007/978-3-319-45541-9_3 . Chapter Google Scholar Miller HP, Bonawitz SC, Ostrovsky O. The effects of delta-9-tetrahydrocannabinol (THC) on inflammation: a review. Cell Immunol. 2020;352: 104111. https://doi.org/10.1016/j.cellimm.2020.104111 . Schurman LD, Lu D, Kendall DA, Howlett AC, Lichtman AH. Molecular mechanism and cannabinoid pharmacology. Handb Exp Pharmacol. 2020;258:323–53. https://doi.org/10.1007/164_2019_298 . Giza CC, Hovda DA. The neurometabolic cascade of concussion. J Athl Train. 2001;36(3):228–35. PubMed PubMed Central Google Scholar Blaylock RL, Maroon J. Immunoexcitotoxicity as a central mechanism in chronic traumatic encephalopathy—a unifying hypothesis. Surg Neurol Int. 2011;2:107. https://doi.org/10.4103/2152-7806.83391 . Bajtel Á, et al. The safety of dronabinol and nabilone: a systematic review and meta-analysis of clinical trials. Pharmaceuticals. 2022;15(1):Art. no. 1. https://doi.org/10.3390/ph15010100 . Nirappil F, Ovalle D, Diamond D. Marijuana reclassification proposed over lower public health risk, documents show. Washington Post, Jan. 13, 2024. [Online]. Available: https://www.washingtonpost.com/health/2024/01/12/marijuana-rescheduling-schedule-3-health-risk/ . Accessed 12 Feb 2024. Crossland BW, et al. Acute supplementation with cannabidiol does not attenuate inflammation or improve measures of performance following strenuous exercise. Healthcare. 2022;10(6):Art. no. 6. https://doi.org/10.3390/healthcare10061133 . Isenmann E, Veit S, Starke L, Flenker U, Diel P. Effects of cannabidiol supplementation on skeletal muscle regeneration after intensive resistance training. Nutrients. 2021;13(9):3028. https://doi.org/10.3390/nu13093028 . Cochrane-Snyman KC, Cruz C, Morales J, Coles M. The effects of cannabidiol oil on noninvasive measures of muscle damage in men. Med Sci Sports Exerc. 2021;53(7):1460–72. https://doi.org/10.1249/MSS.0000000000002606 . Stone WJ, Tolusso DV, Pancheco G, Brgoch S, Nguyen VT. A pilot study on cannabidiol (CBD) and eccentric exercise: impact on inflammation, performance, and pain. Int J Exerc Sci. 2023;16(2):109–17. Raja SN, et al. The revised International Association for the Study of Pain definition of pain: concepts, challenges, and compromises. Pain. 2020;161(9):1976. https://doi.org/10.1097/j.pain.0000000000001939 . Sheffield D, Thornton C, Jones MV. Pain and athletes: Contact sport participation and performance in pain. Psychol Sport Exerc. 2020;49: 101700. https://doi.org/10.1016/j.psychsport.2020.101700 . Park AL, Furie K, Wong SE. Stronger athlete identity is a risk factor for more severe depressive symptoms after musculoskeletal injury in pediatric athletes: a systematic review. Curr Rev Musculoskelet Med. 2023;16(5):220–8. https://doi.org/10.1007/s12178-023-09828-0 . Hill KP, Palastro MD, Johnson B, Ditre JW. Cannabis and pain: a clinical review. Cannabis Cannabinoid Res. 2017;2(1):96–104. https://doi.org/10.1089/can.2017.0017 . Cristino L, Bisogno T, Di Marzo V. Cannabinoids and the expanded endocannabinoid system in neurological disorders. Nat Rev Neurol. 2020;16(1):9–29. https://doi.org/10.1038/s41582-019-0284-z . Committee on the Health Effects of Marijuana: An Evidence Review and Research Agenda, Board on Population Health and Public Health Practice, Health and Medicine Division, and National Academies of Sciences, Engineering, and Medicine, The Health Effects of Cannabis and Cannabinoids: The Current State of Evidence and Recommendations for Research. Washington, D.C.: National Academies Press, 2017, p. 24625. https://doi.org/10.17226/24625 . Whiting PF, et al. Cannabinoids for medical use: a systematic review and meta-analysis. JAMA. 2015;313(24):2456. https://doi.org/10.1001/jama.2015.6358 . Mlost J, Bryk M, Starowicz K. Cannabidiol for pain treatment: focus on pharmacology and mechanism of action. Int J Mol Sci. 2020;21(22):no. 22. https://doi.org/10.3390/ijms21228870 . van de Donk T, Niesters M, Kowal MA, Olofsen E, Dahan A, van Velzen M. An experimental randomized study on the analgesic effects of pharmaceutical-grade cannabis in chronic pain patients with fibromyalgia. Pain. 2019;160(4):860. https://doi.org/10.1097/j.pain.0000000000001464 . Russo M, et al. Evaluating Sativex ® in neuropathic pain management: a clinical and neurophysiological assessment in multiple sclerosis. Pain Med. 2016;17(6):1145–54. https://doi.org/10.1093/pm/pnv080 . Qureshi O, Dua A. COX Inhibitors. In StatPearls , Treasure Island (FL): StatPearls Publishing, 2024. [Online]. Available: http://www.ncbi.nlm.nih.gov/books/NBK549795/ . Accessed 12 Feb 2024. Barakji J, et al. Cannabinoids versus placebo for pain: a systematic review with meta-analysis and trial sequential analysis. PLoS ONE. 2023;18(1): e0267420. https://doi.org/10.1371/journal.pone.0267420 . Nielsen S, et al. Opioid-sparing effect of cannabinoids: a systematic review and meta-analysis. Neuropsychopharmacol. 2017;42(9):1752–65. https://doi.org/10.1038/npp.2017.51 . Webster PC. Medically induced opioid addiction reaching alarming levels. CMAJ. 2012;184(3):285–6. https://doi.org/10.1503/cmaj.109-4088 . M. Azadfard M, M. R. Huecker, and J. M. Leaming, “Opioid Addiction,” in StatPearls , Treasure Island (FL): StatPearls Publishing, 2023. [Online]. Available: http://www.ncbi.nlm.nih.gov/books/NBK448203/ . Accessed 25 Sep 2023. Understanding the Opioid Overdose Epidemic | Opioids | CDC. [Online]. Available: https://www.cdc.gov/opioids/basics/epidemic.html . Accessed 25 Sep 2023. Fischer B, Pang M, Tyndall M. The opioid death crisis in Canada: crucial lessons for public health. The Lancet Public Health. 2019;4(2):e81–2. https://doi.org/10.1016/S2468-2667(18)30232-9 . Pierce M, van Amsterdam J, Kalkman GA, Schellekens A, van den Brink W. Is Europe facing an opioid crisis like the United States? An analysis of opioid use and related adverse effects in 19 European countries between 2010 and 2018. Eur Psychiatry. 2021;64(1): e47. https://doi.org/10.1192/j.eurpsy.2021.2219 . Ekhtiari S, Yusuf I, AlMakadma Y, MacDonald A, Leroux T, Khan M. Opioid use in athletes: a systematic review. Sports Health. 2020;12(6):534–9. https://doi.org/10.1177/1941738120933542 . Cichewicz DL, Martin ZL, Smith FL, Welch SP. Enhancement mu opioid antinociception by oral delta9-tetrahydrocannabinol: dose-response analysis and receptor identification. J Pharmacol Exp Ther. 1999;289(2):859–67. CAS PubMed Google Scholar Cichewicz DL, McCarthy EA. Antinociceptive synergy between delta(9)-tetrahydrocannabinol and opioids after oral administration. J Pharmacol Exp Ther. 2003;304(3):1010–5. https://doi.org/10.1124/jpet.102.045575 . Cox ML, Haller VL, Welch SP. Synergy between delta9-tetrahydrocannabinol and morphine in the arthritic rat. Eur J Pharmacol. 2007;567(1–2):125–30. https://doi.org/10.1016/j.ejphar.2007.04.010 . Smith FL, Cichewicz D, Martin ZL, Welch SP. The enhancement of morphine antinociception in mice by delta9-tetrahydrocannabinol. Pharmacol Biochem Behav. 1998;60(2):559–66. https://doi.org/10.1016/s0091-3057(98)00012-4 . Welch SP, Stevens DL. Antinociceptive activity of intrathecally administered cannabinoids alone, and in combination with morphine, in mice. J Pharmacol Exp Ther. 1992;262(1):10–8. Williams J, Haller VL, Stevens DL, Welch SP. Decreased basal endogenous opioid levels in diabetic rodents: effects on morphine and delta-9-tetrahydrocannabinoid-induced antinociception. Eur J Pharmacol. 2008;584(1):78–86. https://doi.org/10.1016/j.ejphar.2007.12.035 . Salio C, Fischer J, Franzoni MF, Mackie K, Kaneko T, Conrath M. CB1-cannabinoid and mu-opioid receptor co-localization on postsynaptic target in the rat dorsal horn. NeuroReport. 2001;12(17):3689–92. https://doi.org/10.1097/00001756-200112040-00017 . Yu Y, Tsang QK, Jaramillo-Polanco J, Lomax AE, Vanner SJ, Reed DE. Cannabinoid 1 and mu-opioid receptor agonists synergistically inhibit abdominal pain and lack side effects in mice. J Neurosci. 2022;42(33):6313–24. https://doi.org/10.1523/JNEUROSCI.0641-22.2022 . Vázquez M, Guevara N, Maldonado C, Guido PC, Schaiquevich P. Potential pharmacokinetic drug-drug interactions between cannabinoids and drugs used for chronic pain. Biomed Res Int. 2020;2020:3902740. https://doi.org/10.1155/2020/3902740 . Nasrin S, Watson CJW, Perez-Paramo YX, Lazarus P. Cannabinoid metabolites as inhibitors of major hepatic CYP450 enzymes, with implications for cannabis-drug interactions. Drug Metab Dispos. 2021;49(12):1070–80. https://doi.org/10.1124/dmd.121.000442 . Balachandran P, Elsohly M, Hill KP. Cannabidiol interactions with medications, illicit substances, and alcohol: a comprehensive review. J GEN INTERN MED. 2021;36(7):2074–84. https://doi.org/10.1007/s11606-020-06504-8 . Kiraly MA, Kiraly SJ. Traumatic brain injury and delayed sequelae: a review—traumatic brain injury and mild traumatic brain injury (Concussion) are precursors to later-onset brain disorders, including early-onset dementia. Sci World J. 2007;7:1768–76. https://doi.org/10.1100/tsw.2007.269 . Meaney DF, Smith DH. Biomechanics of Concussion. Clin Sports Med. 2011;30(1):19–vii. https://doi.org/10.1016/j.csm.2010.08.009 . Blennow K, Hardy J, Zetterberg H. The neuropathology and neurobiology of traumatic brain injury. Neuron. 2012;76(5):886–99. https://doi.org/10.1016/j.neuron.2012.11.021 . Gardner RC, Yaffe K. Epidemiology of mild traumatic brain injury and neurodegenerative disease. Mol Cell Neurosci. 2015;66:75–80. https://doi.org/10.1016/j.mcn.2015.03.001 . Aychman MM, Goldman DL, Kaplan JS. Cannabidiol’s neuroprotective properties and potential treatment of traumatic brain injuries. Front Neurol. 2023;14:1087011. https://doi.org/10.3389/fneur.2023.1087011 . Magistretti PJ, Allaman I. Lactate in the brain: from metabolic end-product to signalling molecule. Nat Rev Neurosci. 2018;19(4):235–49. https://doi.org/10.1038/nrn.2018.19 . Lactate in the brain: an update on its relevance to brain energy, neurons, glia and panic disorder - Laurel Riske, Rejish K. Thomas, Glen B. Baker, Serdar M. Dursun, 2017. Accessed: Jun. 02, 2024. [Online]. https://doi.org/10.1177/2045125316675579 . Panikashvili D, et al. An endogenous cannabinoid (2-AG) is neuroprotective after brain injury. Nature. 2001;413(6855):Art. no. 6855. https://doi.org/10.1038/35097089 . van der Stelt M, Veldhuis WB, Bär PR, Veldink GA, Vliegenthart JFG, Nicolay K. Neuroprotection by Δ9-tetrahydrocannabinol, the main active compound in marijuana, against ouabain-induced in vivo excitotoxicity. J Neurosci. 2001;21(17):6475–9. https://doi.org/10.1523/JNEUROSCI.21-17-06475.2001 . Naik H, Trojian TH. Therapeutic potential for cannabinoids in sports medicine: current literature review. Curr Sports Med Rep. 2021;20(7):345. https://doi.org/10.1249/JSR.0000000000000858 . Belardo C, et al. Oral cannabidiol prevents allodynia and neurological dysfunctions in a mouse model of mild traumatic brain injury. Front Pharmacol. 2019;10:352. https://doi.org/10.3389/fphar.2019.00352 . Santiago-Castañeda C, Huerta de la Cruz S, Martínez-Aguirre C, Orozco-Suárez SA, Rocha L. Cannabidiol reduces short- and long-term high glutamate release after severe traumatic brain injury and improves functional recovery. Pharmaceutics. 2022;14(8):1609. https://doi.org/10.3390/pharmaceutics14081609 . Bloomfield MAP, et al. The effects of acute cannabidiol on cerebral blood flow and its relationship to memory: An arterial spin labelling magnetic resonance imaging study. J Psychopharmacol. 2020;34(9):981–9. https://doi.org/10.1177/0269881120936419 . Russo EB. Cannabis therapeutics and the future of neurology. Front Integr Neurosci. 2018;12:51. https://doi.org/10.3389/fnint.2018.00051 . Singh J, Neary JP. Neuroprotection following concussion: the potential role for cannabidiol. Can J Neurol Sci. 2020;47(3):289–300. https://doi.org/10.1017/cjn.2020.23 . Schurman LD, Lichtman AH. Endocannabinoids: a promising impact for traumatic brain injury. Front Pharmacol. 2017. https://doi.org/10.3389/fphar.2017.00069 . Young AP, Denovan-Wright EM. The dynamic role of microglia and the endocannabinoid system in neuroinflammation. Front Pharmacol. 2022;12: 806417. https://doi.org/10.3389/fphar.2021.806417 . Kozela E, Pietr M, Juknat A, Rimmerman N, Levy R, Vogel Z. Cannabinoids Δ9-tetrahydrocannabinol and cannabidiol differentially inhibit the lipopolysaccharide-activated NF-κB and interferon-β/STAT proinflammatory pathways in BV-2 microglial cells. J Biol Chem. 2010;285(3):1616–26. https://doi.org/10.1074/jbc.M109.069294 . Tao Y, et al. Cannabinoid receptor-2 stimulation suppresses neuroinflammation by regulating microglial M1/M2 polarization through the cAMP/PKA pathway in an experimental GMH rat model. Brain Behav Immun. 2016;58:118–29. https://doi.org/10.1016/j.bbi.2016.05.020 . Aly E, Khajah MA, Masocha W. β-caryophyllene, a CB2-receptor-selective phytocannabinoid, suppresses mechanical allodynia in a mouse model of antiretroviral-induced neuropathic pain. Molecules. 2019;25(1):106. https://doi.org/10.3390/molecules25010106 . Jha NK, et al. β-caryophyllene, a natural dietary CB2 receptor selective cannabinoid can be a candidate to target the trinity of infection, immunity, and inflammation in COVID-19. Front Pharmacol. 2021;12:321. https://doi.org/10.3389/fphar.2021.590201 . Kalbfell RM, et al. The modulatory role of cannabis use in subconcussive neural injury. iScience. 2023;26(6):106948. https://doi.org/10.1016/j.isci.2023.106948 . Lawrence DW, et al. Cannabis, alcohol and cigarette use during the acute post-concussion period. Brain Inj. 2020;34(1):42–51. https://doi.org/10.1080/02699052.2019.1679885 . Jung T, Hudson R, Rushlow W, Laviolette SR. Functional interactions between cannabinoids, omega-3 fatty acids, and peroxisome proliferator-activated receptors: Implications for mental health pharmacotherapies. Eur J Neurosci. 2022;55(4):1088–100. https://doi.org/10.1111/ejn.15023 . Lago-Fernandez A, Zarzo-Arias S, Jagerovic N, Morales P. Relevance of peroxisome proliferator activated receptors in multitarget paradigm associated with the endocannabinoid system. Int J Mol Sci. 2021;22(3):Art. no. 3. https://doi.org/10.3390/ijms22031001 . McCartney D, Benson MJ, Desbrow B, Irwin C, Suraev A, McGregor IS. Cannabidiol and sports performance: a narrative review of relevant evidence and recommendations for future research. Sports Med - Open. 2020;6(1):27. https://doi.org/10.1186/s40798-020-00251-0 . Dahlgren MK, Lambros AM, Smith RT, Sagar KA, El-Abboud C, Gruber SA. Clinical and cognitive improvement following full-spectrum, high-cannabidiol treatment for anxiety: open-label data from a two-stage, phase 2 clinical trial. Commun Med. 2022;2(1):139. https://doi.org/10.1038/s43856-022-00202-8 . Henson JD, Vitetta L, Hall S. Tetrahydrocannabinol and cannabidiol medicines for chronic pain and mental health conditions. Inflammopharmacol. 2022;30(4):1167–78. https://doi.org/10.1007/s10787-022-01020-z . Penn A. Cannabinoids and mental health, part 2: the search for clinical applications. J Psychosoc Nurs Ment Health Serv. 2019;57(10):7–11. https://doi.org/10.3928/02793695-20190919-02 . Gillman AS, Hutchison KE, Bryan AD. Cannabis and exercise science: a commentary on existing studies and suggestions for future directions. Sports Med. 2015;45(10):1357–63. https://doi.org/10.1007/s40279-015-0362-3 . Docter S, et al. Cannabis use and sport: a systematic review. Sports Health. 2020;12(2):189–99. https://doi.org/10.1177/1941738120901670 . Burr JF, Cheung CP, Kasper AM, Gillham SH, Close GL. Cannabis and athletic performance. Sports Med. 2021;51(Suppl 1):75–87. https://doi.org/10.1007/s40279-021-01505-x . Huestis MA, Mazzoni I, Rabin O. Cannabis in sport: anti-doping perspective. Sports Med. 2011;41(11):949–66. https://doi.org/10.2165/11591430-000000000-00000 . Saugy M, et al. Cannabis and sport. Br J Sports Med. 2006;40 Suppl 1(Suppl 1):i13-15. https://doi.org/10.1136/bjsm.2006.027607 . Kennedy MC. Cannabis: exercise performance and sport. A systematic review. J Sci Med Sport. 2017;20(9):825–9. https://doi.org/10.1016/j.jsams.2017.03.012 . Ware MA, Jensen D, Barrette A, Vernec A, Derman W. Cannabis and the health and performance of the elite athlete. Clin J Sport Med. 2018;28(5):480–4. https://doi.org/10.1097/JSM.0000000000000650 . Charron J, Carey V, Marcotte L’heureux V, Roy P, Comtois AS, Ferland P-M. Acute effects of cannabis consumption on exercise performance: a systematic and umbrella review. J Sports Med Phys Fitness. 2021;61(4):551–61. https://doi.org/10.23736/S0022-4707.20.11003-X . Campos DR, Yonamine M, de Moraed Moreau RL. Marijuana as doping in sports. Sports Med. 2003;33(6):395–9. https://doi.org/10.2165/00007256-200333060-00001 . Ewell TR, Bomar MC, Abbotts KSS, Butterklee HM, Dooley GP, Bell C. Edible marijuana and cycle ergometer exercise. Front Physiol. 2022;13:1085822. https://doi.org/10.3389/fphys.2022.1085822 . Cheung CP, Baker RE, Coates AM, Burr JF. Cannabis containing THC impairs 20-minute cycling time trial performance irrespective of the method of inhalation. J Appl Physiol. 2024. https://doi.org/10.1152/japplphysiol.00757.2023 . Sahinovic A, et al. Effects of cannabidiol on exercise physiology and bioenergetics: a randomised controlled pilot trial. Sports Med - Open. 2022;8(1):27. https://doi.org/10.1186/s40798-022-00417-y . Pinzone AG, Erb EK, Humm SM, Kearney SG, Kingsley JD. Cannabis use for exercise recovery in trained individuals: a survey study. J Cannabis Res. 2023;5(1):32. https://doi.org/10.1186/s42238-023-00198-5 . Gibson LP, Giordano GR, Bidwell LC, Hutchison KE, Bryan AD. Acute effects of ad libitum use of commercially available cannabis products on the subjective experience of aerobic exercise: a crossover study. Sports Med. 2023. https://doi.org/10.1007/s40279-023-01980-4 . Steadward RD, Singh M. The effects of smoking marihuana on physical performance. Med Sci Sports. 1975;7(4):309–11. Avakian EV, Horvath SM, Michael ED, Jacobs S. Effect of marihuana on cardiorespiratory responses to submaximal exercise. Clin Pharmacol Ther. 1979;26(6):777–81. https://doi.org/10.1002/cpt1979266777 . Renaud AM, Cormier Y. Acute effects of marihuana smoking on maximal exercise performance. Med Sci Sports Exerc. 1986;18(6):685–9. Weiss JL, Watanabe AM, Lemberger L, Tamarkin NR, Cardon PV. Cardiovascular effects of delta-9-tetrahydrocannabinol in man. Clin Pharmacol Therap. 1972;13(5part1):671–84. https://doi.org/10.1002/cpt1972135part1671 . Zuurman L, et al. Inhibition of THC-induced effects on the central nervous system and heart rate by a novel CB1 receptor antagonist AVE1625. J Psychopharmacol. 2010;24(3):363–71. https://doi.org/10.1177/0269881108096509 . Kelly TH, Foltin RW, Fischman MW. Effects of smoked marijuana on heart rate, drug ratings and task performance by humans. Behav Pharmacol. 1993;4(2):167–78. D’Souza DC, et al. Blunted psychotomimetic and amnestic effects of delta-9-tetrahydrocannabinol in frequent users of cannabis. Neuropsychopharmacology. 2008;33(10):2505–16. https://doi.org/10.1038/sj.npp.1301643 . Benowitz NL, Jones RT. Prolonged delta-9-tetrahydrocannabinol ingestion. Effects of sympathomimetic amines and autonomic blockades. Clin Pharmacol Ther. 1977;21(3):336–42. https://doi.org/10.1002/cpt1977213336 . Kasper AM, et al. High prevalence of cannabidiol use within male professional rugby union and league players: a quest for pain relief and enhanced recovery. Int J Sport Nutr Exerc Metab. 2020;30(5):315–22. https://doi.org/10.1123/ijsnem.2020-0151 . Peters EN, et al. A randomized, double-blind, placebo-controlled, repeated-dose pilot study of the safety, tolerability, and preliminary effects of a cannabidiol (CBD)- and cannabigerol (CBG)-based beverage powder to support recovery from delayed onset muscle soreness (DOMS). J Int Soc Sports Nutr. 2023;20(1):2280113. https://doi.org/10.1080/15502783.2023.2280113 . Isenmann E, Veit S, Flenker U, Lesch A, Lachenmeier DW, Diel P. Influence of short-term chronic oral cannabidiol application on muscle recovery and performance after an intensive training protocol - a randomized double-blind crossover study. J Int Soc Sports Nutr. 2024;21(1):2337252. https://doi.org/10.1080/15502783.2024.2337252 . Balneaves LG, et al. Canadians’ use of cannabis for therapeutic purposes since legalization of recreational cannabis: a cross-sectional analysis by medical authorization status. BMC Med. 2024;22:150. https://doi.org/10.1186/s12916-024-03370-7 . Balneaves LG, Brown A, Green M. Medical cannabis access and experiences in Canada. 2023. [Online]. Available: www.medicalcannabissurvey.ca . Martinez Naya N, et al. An overview of cannabidiol as a multifunctional drug: pharmacokinetics and cellular effects. Molecules. 2024;29(2):473. https://doi.org/10.3390/molecules29020473 . Lucas CJ, Galettis P, Schneider J. The pharmacokinetics and the pharmacodynamics of cannabinoids. Br J Clin Pharmacol. 2018;84(11):2477–82. https://doi.org/10.1111/bcp.13710 . Huestis MA. Human cannabinoid pharmacokinetics. C&B. 2007;4(8):1770–804. https://doi.org/10.1002/cbdv.200790152 . Chaiton M, Kundu A, Rueda S, Di Ciano P. Are vaporizers a lower-risk alternative to smoking cannabis? Can J Public Health. 2021;113(2):293–6. https://doi.org/10.17269/s41997-021-00565-w . Bidwell LC, Martin-Willett R, Karoly HC. Advancing the science on cannabis concentrates and behavioural health. Drug Alcohol Rev. 2021;40(6):900–13. https://doi.org/10.1111/dar.13281 . Kim J, Choi P, Park Y-T, Kim T, Ham J, Kim J-C. The cannabinoids, CBDA and THCA, rescue memory deficits and reduce amyloid-beta and tau pathology in an Alzheimer’s disease-like mouse model. Int J Mol Sci. 2023;24(7):6827. https://doi.org/10.3390/ijms24076827 . Cheung CP, Coates AM, Millar PJ, Burr JF. Habitual cannabis use is associated with altered cardiac mechanics and arterial stiffness, but not endothelial function in young healthy smokers. J Appl Physiol. 2021;130(3):660–70. https://doi.org/10.1152/japplphysiol.00840.2020 . Williams NNB, et al. Comparison of five oral cannabidiol preparations in adult humans: pharmacokinetics, body composition, and heart rate variability. Pharmaceuticals. 2021;14(1):Art. no. 1. https://doi.org/10.3390/ph14010035 . Moore CF, et al. Pharmacokinetics of oral minor cannabinoids in blood and brain. Cannabis Cannabinoid Res. 2023;8(S1):S51–61. https://doi.org/10.1089/can.2023.0066 . Millar SA, Stone NL, Yates AS, O’Sullivan SE. A systematic review on the pharmacokinetics of cannabidiol in humans. Front Pharmacol. 2018;9:1365. https://doi.org/10.3389/fphar.2018.01365 . Mozaffari K, Willette S, Lucker BF, Kovar SE, Holguin FO, Guzman I. The effects of food on cannabidiol bioaccessibility. Molecules. 2021;26(12):3573. https://doi.org/10.3390/molecules26123573 . Johnson DA, et al. Cannabidiol oil ingested as sublingual drops or within gelatin capsules shows similar pharmacokinetic profiles in healthy males. Cannabis Cannabinoid Res. 2023. https://doi.org/10.1089/can.2023.0117 . Correia-Sá I, Paiva A, Carvalho CM, Vieira-Coelho MA. Cutaneous endocannabinoid system: Does it have a role on skin wound healing bearing fibrosis? Pharmacol Res. 2020;159: 104862. https://doi.org/10.1016/j.phrs.2020.104862 . Sulak D. Handbook of cannabis for clinicians. W.W. Norton & Company; 2021. Google Scholar Brenneisen R, Egli A, Elsohly MA, Henn V, Spiess Y. The effect of orally and rectally administered delta 9-tetrahydrocannabinol on spasticity: a pilot study with 2 patients. Int J Clin Pharmacol Ther. 1996;34(10):446–52. ElSohly MA, Gul W, Walker LA. Pharmacokinetics and tolerability of Δ9-THC-hemisuccinate in a suppository formulation as an alternative to capsules for the systemic delivery of Δ9-THC. Med Cannabis Cannabinoids. 2018;1(1):44–53. https://doi.org/10.1159/000489037 . Bouaziz J, Bar On A, Seidman DS, Soriano D. The clinical significance of endocannabinoids in endometriosis pain management. Cannabis Cannabinoid Res. 2017;2(1):72–80. https://doi.org/10.1089/can.2016.0035 . Rocha MG, Silva JCRe, Ribeiro da Silva A, Candido Dos Reis FJ, Nogueira AA, Poli-Neto OB. TRPV1 expression on peritoneal endometriosis foci is associated with chronic pelvic pain. Reprod Sci. 2011;18(6):511–5. https://doi.org/10.1177/1933719110391279 . Escudero-Lara A, Argerich J, Cabañero D, Maldonado R. Disease-modifying effects of natural Δ9-tetrahydrocannabinol in endometriosis-associated pain. Elife. 2020;9: e50356. https://doi.org/10.7554/eLife.50356 . Spindle TR, et al. Cannabinoid content and label accuracy of hemp-derived topical products available online and at national retail stores. JAMA Netw Open. 2022;5(7): e2223019. https://doi.org/10.1001/jamanetworkopen.2022.23019 . Gidal BE, et al. Product labeling accuracy and contamination analysis of commercially available cannabidiol product samples. Front Pharmacol. 2024;15:1335441. https://doi.org/10.3389/fphar.2024.1335441 . Johnson E, Kilgore M, Babalonis S. Label accuracy of unregulated cannabidiol (CBD) products: measured concentration vs. label claim. J Cannabis Res. 2022;4:28. https://doi.org/10.1186/s42238-022-00140-1 . Watkins PB, Church RJ, Li J, Knappertz V. Cannabidiol and abnormal liver chemistries in healthy adults: results of a phase I clinical trial. Clin Pharmacol Ther. 2021;109(5):1224–31. https://doi.org/10.1002/cpt.2071 . Feng S, Mäntymäki M, Dhir A, Salmela H. How Self-tracking and the quantified self promote health and well-being: systematic review. J Med Internet Res. 2021;23(9): e25171. https://doi.org/10.2196/25171 . Patel J, Marwaha R. Cannabis use disorder. In StatPearls , Treasure Island (FL): StatPearls Publishing, 2024. [Online]. Available: http://www.ncbi.nlm.nih.gov/books/NBK538131/ . Accessed 25 May 2024. National Academies of Sciences E, Division HM, B. Practice PHPH, C. on the H. E. of M. A. E. R. and R. Agenda. Problem cannabis use. In: The Health Effects of Cannabis and Cannabinoids: The Current State of Evidence and Recommendations for Research, National Academies Press (US), 2017. [Online]. Available: https://www.ncbi.nlm.nih.gov/books/NBK425740/ . Accessed 25 May 2024. Lapham GT, et al. Prevalence of cannabis use disorder and reasons for use among adults in a US State where recreational cannabis use is legal. JAMA Netw Open. 2023;6(8): e2328934. https://doi.org/10.1001/jamanetworkopen.2023.28934 . Compton WM, Han B, Jones CM, Blanco C. Cannabis use disorders among adults in the United States during a time of increasing use of cannabis. Drug Alcohol Depend. 2019;204: 107468. https://doi.org/10.1016/j.drugalcdep.2019.05.008 . Zeiger JS, Silvers WS, Fleegler EM, Zeiger RS. Cannabis use in active athletes: behaviors related to subjective effects. PLoS ONE. 2019;14(6): e0218998. https://doi.org/10.1371/journal.pone.0218998 . Cannabis Removed from In-Competition Analysis for Student-Athlete Samples | Canadian Centre for Ethics in Sport. [Online]. Available: https://cces.ca/news/cannabis-removed-competition-analysis-student-athlete-samples . Accessed 16 Apr. 2023. Jaeger K. NCAA Panel Recommends Removing Marijuana From Banned Substances List For College Athletes. Marijuana Moment. [Online]. Available: https://www.marijuanamoment.net/ncaa-panel-recommends-removing-marijuana-from-banned-substances-list-for-college-athletes/ . Accessed 9 Oct 2023. “NCAA Council Votes to Remove Cannabis From Banned Drug List, Removes Limits on On-Field Coaches,” US News & World Report. [Online]. Available: // www.usnews.com/news/sports/articles/2024-06-25/ncaa-council-votes-to-remove-cannabis-from-banned-drug-list-removes-limits-on-on-field-coaches . Accessed 8 Jul 2024. 2023list_explanatory_list_en_final_26_september_2022.pdf. [Online]. Available: https://www.wada-ama.org/sites/default/files/2022-09/2023list_explanatory_list_en_final_26_september_2022.pdf . Accessed 27 May 2024. About Us | Certified for Sport®. [Online]. Available: https://www.nsfsport.com/about-us/ . Accessed 11 Oct 2023. Evanoff AB, Quan T, Dufault C, Awad M, Bierut LJ. Physicians-in-training are not prepared to prescribe medical marijuana. Drug Alcohol Depend. 2017;180:151–5. https://doi.org/10.1016/j.drugalcdep.2017.08.010 . Patel S, Doroudgar S, Ip EJ. Community pharmacists’ lack of knowledge and confidence in non-prescription cannabidiol products. Res Social Adm Pharm. 2021;17(7):1356–60. https://doi.org/10.1016/j.sapharm.2020.09.015 . Canada and Health Canada, Information for health care professionals: cannabis (marihuana, marijuana) and the cannabinoids : dried or fresh plant and oil administration by ingestion or other means psychoactive agent. 2018. [Online]. Available: http://publications.gc.ca/collections/collection_2018/sc-hc/H129-19-2018-eng.pdf . Accessed 16 Oct 2021. Berlekamp D, Rao PSS, Patton T, Berner J. Surveys of pharmacy students and pharmacy educators regarding medical marijuana. Curr Pharm Teach Learn. 2019;11(7):669–77. https://doi.org/10.1016/j.cptl.2019.03.006 . Isralowitz R, Temple LM, Zolotov Y, Kogan M. CTIM editors’ commentary: Special issue on medical cannabis in professional education. Complement Ther Med. 2021;63: 102786. https://doi.org/10.1016/j.ctim.2021.102786 . “Cannabis Regulations Inadequate Given Rising Health Risks of High-Potency Products,” USC Schaeffer. [Online]. Available: https://healthpolicy.usc.edu/article/cannabis-regulations-inadequate-given-rising-health-risks-of-high-potency-products/ . Accessed 30 Oct 2023. “Insurance Coverage for Medical Cannabis in Canada,” Medical Marijuana Consulting. [Online]. Available: https://medmc.ca/resource/insurance-coverage-for-medical-cannabis/ . Accessed 10 Oct 2023. United States Patent and Trademark Office. [Online]. Available: https://assignment.uspto.gov/patent/index.html#/patent/search/resultAbstract?id=9895342&type=patNum . Accessed 10 Oct 2023. Download references AcknowledgementsWe would like to acknowledge the University of Saskatchewan and the University of Regina for their support. This work was partially funded by the National Football League (NFL-NFLPA) Pain Management Committee (PMC) research grant. The authors have no competing interests to declare. Author informationAuthors and affiliations. University of Saskatchewan, Saskatoon, SK, S7N 5E5, Canada Elizabeth S. Thompson & Jane Alcorn University of Regina, Regina, SK, S4S 0A2, Canada J. Patrick Neary You can also search for this author in PubMed Google Scholar Corresponding authorCorrespondence to Elizabeth S. Thompson . Ethics declarationsPartially funded by a National Football League (NFL-NFLPA) Pain Management Committee (PMC) research grant. Author ContributionsEST: writing—original draft, conceptualization, investigation, formal analysis, and writing—review & editing. JPN: supervision, conceptualization, funding acquisition, project administration, and writing—review & editing. JA: supervision, conceptualization, funding acquisition, project administration, and writing—review & editing. All authors read and approved the final version. Conflicts of Interest/Competing InterestsElizabeth S. Thompson is a member of the Society of Cannabis Clinicians and the International Society to Advance Alzheimer’s Research and Treatment (ISTAART). No compensation is received as member. Jane Alcorn and J. Patrick Neary declare no conflicts of interest that are directly relevant to the content of this article. ChatGPT 3.5 was used to assist with refining grammar and sentence structure. We affirm that all ideas, analyses, arguments, and conclusions in this paper are entirely our own original work. ChatGPT was not used to generate content, conduct research, or contribute to the substantive elements of this paper and served solely as a grammatical assistant. This declaration is made in the interest of transparency and in compliance with current academic practices regarding the use of AI tools in research writing. Availability of Data and MaterialsNot applicable. Ethics ApprovalInformed consent. 11-Hydroxy-Δ9-tetrahydrocannabinol. 2 arachidonoyl-glycerol. 2-monoacyl-glycerol. 5-hydroxytryptamine receptor 1A. Association of American Medical Colleges. Amyloid beta proteins. Arachidonoylethanolamide or anandamide Brain derived neurotrophic factor. Calcium ion. Cannabinoid receptor type 1. Cannabinoid receptor type 2. Cannabidiol. Cannabidiolic acid. Canadian Collegiate Athletic Association. Center for Disease Control and Prevention. Central nervous system. 11-nor-9-carboxy-Δ9-tetrahydrocannabinol Cyclooxygenase-2. Chronic traumatic encephalopathy. Drug Enforcement Administration. Endocannabinoid system. Effective dose 50%. Fatty acid amide hydrolase. Food and drug administration. G-protein coupled receptors. US Department of Health and Human Services. Health spending account. Interleukin-10. Interleukin-1β. Interleukin-6. Inducible nitric oxide synthase. Monoacylglycerol lipase. Major League Baseball. Matrix Metalloproteinase-9. Medial prefrontal cortex. Multiple sclerosis. Mild traumatic brain injury. Nucleus accumbens. N-acylethanolamine. National Basketball League. National Collegiate Athletics Association. Nuclear factor-kappaB. National Football League. N -methyl- d -aspartate. Nonsteroidal anti-inflammatory drugs.. National Sanitation Foundation. Polymorphonuclear neutrophils. Peroxisome proliferator-activated receptors. Reactive oxygen species. S100 calcium-binding protein B. Transforming Growth Factor Beta-1. Δ9-tetrahydrocannabinol. Tetrahydrocannabinol-hemisuccinate. Tetrahydrocannabinolic acid. Tumor necrosis factor alpha. Transient receptor potential ion channels. Vascular endothelial growth factor. Ventral tegmental area. World Anti-Doping Agency. Rights and permissionsSpringer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law. Reprints and permissions About this articleThompson, E.S., Alcorn, J. & Neary, J.P. Cannabinoid Therapy in Athletics: A Review of Current Cannabis Research to Evaluate Potential Real-World Cannabinoid Applications in Sport. Sports Med (2024). https://doi.org/10.1007/s40279-024-02094-1 Download citation Accepted : 31 July 2024 Published : 21 August 2024 DOI : https://doi.org/10.1007/s40279-024-02094-1 Share this articleAnyone you share the following link with will be able to read this content: Sorry, a shareable link is not currently available for this article. Provided by the Springer Nature SharedIt content-sharing initiative - Find a journal
- Publish with us
- Track your research
 |




























IMAGES
COMMENTS
The American Journal of Sports Medicine, founded in 1972, is the official publication of the American Orthopaedic Society for Sports Medicine.It contains original articles addressed to orthopaedic surgeons specializing in sports medicine, and to team physicians, athletic trainers, and physical therapists focusing on the causes and effects of injury or disease resulting from or affected by ...
Research in Sports Medicine is a broad journal that aims to bridge the gap between all professionals in the fields of sports medicine. The journal serves an international audience and is of interest to professionals worldwide. The journal covers major aspects of sports medicine and sports science - prevention, management, and rehabilitation of sports, exercise and physical activity related ...
Incidence and burden of 671 injuries in professional women footballers: time to focus on context-specific injury risk reduction strategies. Olivier Materne et al. Published online: 19 Jun 2024. Explore the current issue of Research in Sports Medicine, Volume 32, Issue 5, 2024.
British Journal of Sports Medicine (BJSM) is a Plan S compliant Transformative Journal. British Journal of Sports Medicine (BJSM) is a multimedia portal for authoritative original research, systematic reviews, consensus statements and debate in sport and exercise medicine (SEM). We define sport and exercise medicine broadly. BJSM's web, print, video and audio material serves the ...
The American Journal of Sports Medicine (AJSM) is the official peer-reviewed scientific journal of the American Orthopaedic Society for Sports Medicine (AOSSM). Founded in 1972, AJSM is an essential forum for independent orthopaedic sports medicine research and education, allowing clinical practitioners the ability to make decisions based on sound scientific information.
Sports Medicine also welcomes the submission of high-quality original research in the above fields. As a hybrid journal, Sports Medicine does not charge authors to publish using the traditional subscription-based publishing route, but does offer the option to publish accepted articles open access if authors so wish or if their funders require ...
Aims and scope. Sports Medicine - Open focuses on original research and definitive reviews in the field of sport and exercise medicine. The Journal includes medical and scientific research relating to: Sporting performance enhancement including nutrition, equipment and training. Medical syndromes associated with sport and exercise.
The purpose of the Sports Medicine and Health Science (SMHS) journal is to provide a scientific, merit-based, high-quality publication platform for all relevant biomedical studies worldwide with a primary focus on sports medicine, physical activity, and the exercise-related health sciences. The …. View full aims & scope.
Current Sports Medicine Reports is unique in its focus entirely on the clinical aspects of sports medicine. This peer-reviewed journal harnesses the tremendous scientific and clinical resources of ACSM to develop articles reviewing recent and important advances in the field that have clinical relevance. The journal's goal is to translate the latest research and advances in the field into ...
Sports Health: A Multidisciplinary Approach (SPH) is a bi-monthly, peer-reviewed journal for primary care physicians, orthopaedic surgeons, physical therapists, athletic trainers and other medical and health care professionals involved in the training and care of the competitive or recreational athlete.SPH publishes review articles, original research articles, case studies, images, short ...
Aritra Majumdar, Rashid Bakirov and Tim Rees. Sports Medicine - Open 2024 10 :85. Letter Published on: 29 July 2024. The original article was published in Sports Medicine - Open 2024 10 :84. The Leading Article to this article has been published in Sports Medicine - Open 2022 8 :73. Full Text.
David Rhodes. Damian J. Harper. Systematic Review Open access 14 May 2024 Pages: 2109 - 2139. 1. 2. …. 79. Next. Sports Medicine bridges the gap between science and practice in the promotion of exercise and health, and in the scientific assessment, study and ...
As injury is an inevitable part of sports participation, more and more attention has been paid to the research of sports medicine. Due to the rapid growth of sports medicine of athletes research, it is a challenge to entirely understand its research status and hotspots. ... Marx W. HistCite analysis of papers constituting the h index research ...
Journal of Sports Science and Medicine. Journal of Sports Science and Medicine (JSSM) is a nonprofit scientific electronic journal, publishing research and case studies, and review article in the fields of sports medicine and exercise sciences. JSSM is an open access journal which means that all content is freely available without charge to the ...
As such, optimising performance, improving the best players' availability, and decreasing the risk of injury have become the main thrusts of sports science and sports medicine when tied to high-performance teams. 5. Sports science research can help lead to evidence-based approaches that will allow athletes and active individuals to exercise ...
Research in Sports Medicine is a broad journal that aims to bridge the gap between all professionals in the fields of sports medicine. The journal serves an international audience and is of interest to professionals worldwide. The journal covers major aspects of sports medicine and sports science - prevention, management, and rehabilitation of sports, exercise and physical activity related ...
Sports Medicine focuses on definitive and comprehensive review articles that interpret and evaluate the current literature to provide the rationale for and application of research findings in the sports medicine and exercise field. Major topics covered by reviews published in the journal include: Sports medicine and sports science, including performance research.
Orthopedic sports medicine continues to evolve, owing much of its clinical management and practice to rigorous academic research. In this review, we identify and describe the top 100 cited articles in clinical sports medicine and recognize the authors and institutions driving the research. We collec …
Sports Medicine is a relatively new topic in medicine and includes a variety of medical and paramedical fields. Although sports medicine is mistakenly thought to be mainly for sports professionals/athletes, it actually encompasses the entire population, including the active and non-active healthy populations, as well as the sick [].Sports medicine also engages amateur sportsmen and strives to ...
Volume 10 2001. Volume 9 1999-2000. Volume 8 1998. Volume 7 1996-1997. Volume 6 1995-1996. Volume 5 1994-1995. Volume 4 1993. Volume 3 1991-1992. Volume 2 1990-1991.
In 2020, Medicine & Science in Sports & Exercise® ( MSSE®) published 304 articles, amounting to 2,690 pages of text. These articles were published out of approximately 1,300 submissions at an acceptance rate of 24.6%. As expected of the American College of Sports Medicine's (ACSM) flagship journal, the scientific content of these articles ...
Together, research shows that organized sports, in clubs or companies, are more important for people's overall physical activity than ever before. Groups that are usually less physically active can be motivated through sport—for example, elderly men in sport supporters' clubs [ 169 ], people in rural areas [ 170 ], migrants [ 171 ], and ...
Using power analysis to estimate appropriate sample size. The main aim of this paper is to provide some practical guidance to researchers on how statistical power analysis can be used to estimate sample size in empirical design. The paper describes the key assumptions underlying statistical... more. Download.
The increasing legalization of Cannabis sativa plant products has sparked growing interest in their therapeutic applications. Prohibition laws established in 1937 hindered formal research on cannabis, a plant with cultural and medicinal roots dating back to 2700 BC in Chinese history. Despite regulatory hurdles, published research on cannabis has emerged; yet elite athletes remain an ...
The public policy chaos fueled by the June 2022 Dobbs v Jackson Women's Health Organization Supreme Court decision has created a critical need for objective and high-quality abortion policy evaluation research. Stevenson and Root 1 rose to this challenge by conducting a convincing analysis of recent trends in maternal mortality, motivated in part by pro-life advocate claims that the recent ...